Our body naturally produces as much as 10,000 IU of vitamin D based on a few minutes of sun exposure when the sun is high. Getting that much vitamin D from dietary sources is very difficult, even after “fortification”.
The above refers to pre-sunburn exposure. Sunburn is not associated with increased vitamin D production; it is associated with skin damage and cancer.
Solar ultraviolet (UV) radiation is generally divided into two main types: UVB (wavelength: 280–320 nm) and UVA (320–400 nm). Vitamin D is produced primarily based on UVB radiation. Nevertheless, UVA is much more abundant, amounting to about 90 percent of the sun’s UV radiation.
UVA seems to cause the most skin damage, although there is some debate on this. If this is correct, one would expect skin pigmentation to be our body’s defense primarily against UVA radiation, not UVB radiation. If so, one’s ability to produce vitamin D based on UVB should not go down significantly as one’s skin becomes darker.
Also, vitamin D and cholesterol seem to be closely linked. Some argue that one is produced based on the other; others that they have the same precursor substance(s). Whatever the case may be, if vitamin D and cholesterol are indeed closely linked, one would expect low cholesterol levels to be associated with low vitamin D production based on sunlight.
Bogh et al. (2010) recently published a very interesting study. The link to the study was provided by Ted Hutchinson in the comments sections of a previous post on vitamin D. (Thanks Ted!) The study was published in a refereed journal with a solid reputation, the Journal of Investigative Dermatology.
The study by Bogh et al. (2010) is particularly interesting because it investigates a few issues on which there is a lot of speculation. Among the issues investigated are the effects of total cholesterol and skin pigmentation on the production of vitamin D from UVB radiation.
The figure below depicts the relationship between total cholesterol and vitamin D production based on UVB radiation. Vitamin D production is referred to as “delta 25(OH)D”. The univariate correlation is a fairly high and significant 0.51.
25(OH)D is the abbreviation for calcidiol, a prehormone that is produced in the liver based on vitamin D3 (cholecalciferol), and then converted in the kidneys into calcitriol, which is usually abbreviated as 1,25-(OH)2D3. The latter is the active form of vitamin D.
The table below shows 9 columns; the most relevant ones are the last pair at the right. They are the delta 25(OH)D levels for individuals with dark and fair skin after exposure to the same amount of UVB radiation. The difference in vitamin D production between the two groups is statistically indistinguishable from zero.
So there you have it. According to this study, low total cholesterol seems to be associated with impaired ability to produce vitamin D from UVB radiation. And skin pigmentation appears to have little effect on the amount of vitamin D produced.
I hope that there will be more research in the future investigating this study’s claims, as the study has a few weaknesses. For example, if you take a look at the second pair of columns from the right on the table above, you’ll notice that the baseline 25(OH)D is lower for individuals with dark skin. The difference was just short of being significant at the 0.05 level.
What is the problem with that? Well, one of the findings of the study was that lower baseline 25(OH)D levels were significantly associated with higher delta 25(OH)D levels. Still, the baseline difference does not seem to be large enough to fully explain the lack of difference in delta 25(OH)D levels for individuals with dark and fair skin.
A widely cited dermatology researcher, Antony Young, published an invited commentary on this study in the same journal issue (Young, 2010). The commentary points out some weaknesses in the study, but is generally favorable. The weaknesses include the use of small sub-samples.
References
Bogh, M.K.B., Schmedes, A.V., Philipsen, P.A., Thieden, E., & Wulf, H.C. (2010). Vitamin D production after UVB exposure depends on baseline vitamin D and total cholesterol but not on skin pigmentation. Journal of Investigative Dermatology, 130(2), 546–553.
Young, A.R. (2010). Some light on the photobiology of vitamin D. Journal of Investigative Dermatology, 130(2), 346–348.
Monday, February 28, 2011
Thursday, February 24, 2011
Polyphenols, Hormesis and Disease: Part II
In the last post, I explained that the body treats polyphenols as potentially harmful foreign chemicals, or "xenobiotics". How can we reconcile this with the growing evidence that at least a subset of polyphenols have health benefits?
Clues from Ionizing Radiation
One of the more curious things that has been reported in the scientific literature is that although high-dose ionizing radiation (such as X-rays) is clearly harmful, leading to cancer, premature aging and other problems, under some conditions low-dose ionizing radiation can actually decrease cancer risk and increase resistance to other stressors (1, 2, 3, 4, 5). It does so by triggering a protective cellular response, increasing cellular defenses out of proportion to the minor threat posed by the radiation itself. The ability of mild stressors to increase stress resistance is called "hormesis." Exercise is a common example. I've written about this phenomenon in the past (6).
The Case of Resveratrol
Resveratrol is perhaps the most widely known polyphenol, available in supplement stores nationwide. It's seen a lot of hype, being hailed as a "calorie restriction mimetic" and the reason for the "French paradox."* But there is quite a large body of evidence suggesting that resveratrol functions in the same manner as low-dose ionizing radiation and other bioactive polyphenols: by acting as a mild toxin that triggers a hormetic response (7). Just as in the case of radiation, high doses of resveratrol are harmful rather than helpful. This has obvious implications for the supplementation of resveratrol and other polyphenols. A recent review article on polyphenols stated that while dietary polyphenols may be protective, "high-dose fortified foods or dietary supplements are of unproven efficacy and possibly harmful" (8).
The Cellular Response to Oxidants
Although it may not be obvious, radiation and polyphenols activate a cellular response that is similar in many ways. Both activate the transcription factor Nrf2, which activates genes that are involved in detoxification of chemicals and antioxidant defense**(9, 10, 11, 12). This is thought to be due to the fact that polyphenols, just like radiation, may temporarily increase the level of oxidative stress inside cells. Here's a quote from the polyphenol review article quoted above (13):
Nrf2 is one of the main pathways by which polyphenols increase stress resistance and antioxidant defenses, including the key cellular antioxidant glutathione (14). Nrf2 activity is correlated with longevity across species (15). Inducing Nrf2 activity via polyphenols or by other means substantially reduces the risk of common lifestyle disorders in animal models, including cardiovascular disease, diabetes and cancer (16, 17, 18), although Nrf2 isn't necessarily the only mechanism. The human evidence is broadly consistent with the studies in animals, although not as well developed.
One of the most interesting effects of hormesis is that exposure to one stressor can increase resistance to other stressors. For example, long-term consumption of high-polyphenol chocolate increases sunburn resistance in humans, implying that it induces a hormetic response in skin (19). Polyphenol-rich foods such as green tea reduce sunburn and skin cancer development in animals (20, 21).
Chris Masterjohn first introduced me to Nrf2 and the idea that polyphenols act through hormesis. Chris studies the effects of green tea on health, which seem to be mediated by polyphenols.
A Second Mechanism
There is a place in the body where polyphenols are concentrated enough to be direct antioxidants: in the digestive tract after consuming polyphenol-rich foods. Digestion is a chemically harsh process that readily oxidizes ingested substances such as polyunsaturated fats (22). Oxidized fat is neither healthy when it's formed in the deep fryer, nor when it's formed in the digestive tract (23, 24). Eating polyphenol-rich foods effectively prevents these fats from being oxidized during digestion (25). One consequence of this appears to be better absorption and assimilation of the exceptionally fragile omega-3 polyunsaturated fatty acids (26).
What does it all Mean?
I think that overall, the evidence suggests that polyphenol-rich foods are healthy in moderation, and eating them on a regular basis is generally a good idea. Certain other plant chemicals, such as suforaphane found in cruciferous vegetables, and allicin found in garlic, exhibit similar effects and may also act by hormesis (27). Some of the best-studied polyphenol-rich foods are tea (particularly green tea), blueberries, extra-virgin olive oil, red wine, citrus fruits, hibiscus tea, soy, dark chocolate, coffee, turmeric and other herbs and spices, and a number of traditional medicinal herbs. A good rule of thumb is to "eat the rainbow", choosing foods with a variety of colors.
Supplementing with polyphenols and other plant chemicals in amounts that would not be achievable by eating food is probably not a good idea.
* The "paradox" whereby the French eat a diet rich in saturated fat, yet have a low heart attack risk compared to other affluent Western nations.
** Genes containing an antioxidant response element (ARE) in the promoter region. ARE is also sometimes called the electrophile response element (EpRE).
Clues from Ionizing Radiation
One of the more curious things that has been reported in the scientific literature is that although high-dose ionizing radiation (such as X-rays) is clearly harmful, leading to cancer, premature aging and other problems, under some conditions low-dose ionizing radiation can actually decrease cancer risk and increase resistance to other stressors (1, 2, 3, 4, 5). It does so by triggering a protective cellular response, increasing cellular defenses out of proportion to the minor threat posed by the radiation itself. The ability of mild stressors to increase stress resistance is called "hormesis." Exercise is a common example. I've written about this phenomenon in the past (6).
The Case of Resveratrol
Resveratrol is perhaps the most widely known polyphenol, available in supplement stores nationwide. It's seen a lot of hype, being hailed as a "calorie restriction mimetic" and the reason for the "French paradox."* But there is quite a large body of evidence suggesting that resveratrol functions in the same manner as low-dose ionizing radiation and other bioactive polyphenols: by acting as a mild toxin that triggers a hormetic response (7). Just as in the case of radiation, high doses of resveratrol are harmful rather than helpful. This has obvious implications for the supplementation of resveratrol and other polyphenols. A recent review article on polyphenols stated that while dietary polyphenols may be protective, "high-dose fortified foods or dietary supplements are of unproven efficacy and possibly harmful" (8).
The Cellular Response to Oxidants
Although it may not be obvious, radiation and polyphenols activate a cellular response that is similar in many ways. Both activate the transcription factor Nrf2, which activates genes that are involved in detoxification of chemicals and antioxidant defense**(9, 10, 11, 12). This is thought to be due to the fact that polyphenols, just like radiation, may temporarily increase the level of oxidative stress inside cells. Here's a quote from the polyphenol review article quoted above (13):
We have found that [polyphenols] are potentially far more than 'just antioxidants', but that they are probably insignificant players as 'conventional' antioxidants. They appear, under most circumstances, to be just the opposite, i.e. prooxidants, that nevertheless appear to contribute strongly to protection from oxidative stress by inducing cellular endogenous enzymic protective mechanisms. They appear to be able to regulate not only antioxidant gene transcription but also numerous aspects of intracellular signaling cascades involved in the regulation of cell growth, inflammation and many other processes.It's worth noting that this is essentially the opposite of what you'll hear on the evening news, that polyphenols are direct antioxidants. The scientific cutting edge has largely discarded that hypothesis, but the mainstream has not yet caught on.
Nrf2 is one of the main pathways by which polyphenols increase stress resistance and antioxidant defenses, including the key cellular antioxidant glutathione (14). Nrf2 activity is correlated with longevity across species (15). Inducing Nrf2 activity via polyphenols or by other means substantially reduces the risk of common lifestyle disorders in animal models, including cardiovascular disease, diabetes and cancer (16, 17, 18), although Nrf2 isn't necessarily the only mechanism. The human evidence is broadly consistent with the studies in animals, although not as well developed.
One of the most interesting effects of hormesis is that exposure to one stressor can increase resistance to other stressors. For example, long-term consumption of high-polyphenol chocolate increases sunburn resistance in humans, implying that it induces a hormetic response in skin (19). Polyphenol-rich foods such as green tea reduce sunburn and skin cancer development in animals (20, 21).
Chris Masterjohn first introduced me to Nrf2 and the idea that polyphenols act through hormesis. Chris studies the effects of green tea on health, which seem to be mediated by polyphenols.
A Second Mechanism
There is a place in the body where polyphenols are concentrated enough to be direct antioxidants: in the digestive tract after consuming polyphenol-rich foods. Digestion is a chemically harsh process that readily oxidizes ingested substances such as polyunsaturated fats (22). Oxidized fat is neither healthy when it's formed in the deep fryer, nor when it's formed in the digestive tract (23, 24). Eating polyphenol-rich foods effectively prevents these fats from being oxidized during digestion (25). One consequence of this appears to be better absorption and assimilation of the exceptionally fragile omega-3 polyunsaturated fatty acids (26).
What does it all Mean?
I think that overall, the evidence suggests that polyphenol-rich foods are healthy in moderation, and eating them on a regular basis is generally a good idea. Certain other plant chemicals, such as suforaphane found in cruciferous vegetables, and allicin found in garlic, exhibit similar effects and may also act by hormesis (27). Some of the best-studied polyphenol-rich foods are tea (particularly green tea), blueberries, extra-virgin olive oil, red wine, citrus fruits, hibiscus tea, soy, dark chocolate, coffee, turmeric and other herbs and spices, and a number of traditional medicinal herbs. A good rule of thumb is to "eat the rainbow", choosing foods with a variety of colors.
Supplementing with polyphenols and other plant chemicals in amounts that would not be achievable by eating food is probably not a good idea.
* The "paradox" whereby the French eat a diet rich in saturated fat, yet have a low heart attack risk compared to other affluent Western nations.
** Genes containing an antioxidant response element (ARE) in the promoter region. ARE is also sometimes called the electrophile response element (EpRE).
Monday, February 21, 2011
The China Study II: Wheat, dietary fat, and mortality
In this post on the China Study II data we have seen that wheat apparently displaces dietary fat a lot, primarily fat from animal sources. We have also seen in that post that wheat is strongly and positively associated with mortality in both the 35-69 and 70-79 age ranges, whereas dietary fat is strongly and negatively associated with mortality in those ranges.
This opens the door for the hypothesis that wheat increased mortality in the China Study II sample mainly by displacing dietary fat, and not necessarily by being a primary cause of health problems. In fact, given the strong displacement effect discussed in the previous post, I thought that this hypothesis was quite compelling. I was partly wrong, as you’ll see below.
A counterintuitive hypothesis no doubt, given that wheat is unlikely to have been part of the diet of our Paleolithic ancestors, and thus the modern human digestive tract may be maladapted to it. Moreover, wheat’s main protein (gluten) is implicated in celiac disease, and wheat contains plant toxins such as wheat germ agglutinin.
Still, we cannot completely ignore this hypothesis because: (a) the data points in its general direction; and (b) wheat-based foods are found in way more than trivial amounts in the diets of populations that have relatively high longevity, such as the French.
Testing the hypothesis essentially amounts to testing the significance of two mediating effects; of fat as a mediator of the effects of wheat on mortality, in both the 35-69 and 70-79 age ranges. There are two main approaches for doing this. One is the classic test discussed by Baron & Kenny (1986). The other is the modern test discussed by Preacher & Hayes (2004), and extended by Hayes & Preacher (2010) for nonlinear relationships.
I tested the meditating effects using both approaches, including the nonlinear variation. I used the software WarpPLS for this; the results below are from WarpPLS outputs. Other analyses of the China Study data using WarpPLS can be found here (calorie restriction and longevity), and here (wheat, rice, and cardiovascular disease). For yet other studies, click here.
The graphs below show the path coefficients and chance probabilities of two models. The one at the top-left suggests that wheat flour consumption seems to be associated with a statistically significant increase in mortality in the 70-79 age range (beta=0.23; P=0.04). The effect in the 35-69 age range is almost statistically significant (beta=0.22; P=0.09); the likelihood that it is due to chance is 9 percent (this is the meaning of the P=0.09=9/100=9%).
The graph at the bottom-right suggests that the variable “FatCal”, which is the percentage of calories coming from dietary fat, is indeed a significant mediator of the relationships above between wheat and mortality, in both ranges. But “FatCal” is only a partial mediator.
The reason why “FatCal” is not a “perfect” mediator is that the direct effects of wheat on mortality in both ranges are still relatively strong after “FatCal” is added to the model (i.e., controlled for). In fact, the effects of wheat on mortality don’t change that much with the introduction of the variable “FatCal”.
This analysis suggests that, in the China Study II sample, one of wheat’s main sins might indeed have been to displace dietary fat from animal sources. Wheat consumption is strongly and negatively associated with dietary fat (beta=-0.37; P<0.01), and dietary fat is relatively strongly and negatively associated with mortality in both ranges (more in the 70-79 age range).
Why is dietary fat more protective in the 70-79 than in the 35-69 age range, with the latter effect only being significant at the P=0.10 level (a 10 percent chance probability)? My interpretation is that, as with almost any dietary habit, it takes years for a chronically low fat diet to lead to problems. See graph below; fat was not a huge contributor to the total calorie intake in this sample.
The analysis suggests that wheat also caused problems via other paths. What are them? We can’t say for sure based on this dataset. Perhaps the paths involve lectins and/or gluten. One way or another, the relationship is complex. As you can see from the graph below, the relationship between wheat consumption and mortality is nonlinear for the 70-79 age range, most likely due to confounding factors. The effect size is small for the 35-69 age range, even though it looks linear or quasi-linear in that range.
As you might recall from this post, rice does NOT displace dietary fat, and it seems to be associated with increased longevity. Carbohydrate content per se does not appear to be the problem here. Both rice and wheat foods are rich in them, and have a high glycemic index. Wheat products tend to have a higher glycemic load though.
And why is dietary fat so important as to be significantly associated with increased longevity? This is not a trivial question, because if too much of that fat is stored as body fat it will actually decrease longevity. Dietary fat is very calorie-dense, and can be easily stored as body fat.
Dietary fat is important for various reasons, and probably some that we don’t know about yet. It leads to the formation of body fat, which is not only found in adipocytes or used only as a store of energy. Fat is a key component of a number of important tissues, including 60 percent of our brain. Since fat in the human body undergoes constant turnover, more in some areas than others, lack of dietary fat may compromise the proper functioning of various organs.
Without dietary fat, the very important fat-soluble vitamins (A, D, E and K) cannot be properly absorbed. Taking these vitamins in supplemental form will not work if you don’t consume fat as well. A very low fat diet is almost by definition a diet deficient in fat-soluble vitamins, even if those vitamins are consumed in large amounts via supplements.
Moreover, animals store fat-soluble vitamins in their body fat (as well as in organs), so we get these vitamins in one of their most natural and potent forms when we consume animal fat. Consuming copious amounts of olive and/or coconut oil will not have just the same effect.
References
Baron, R. M., & Kenny, D. A. (1986). The moderator–mediator variable distinction in social psychological research: Conceptual, strategic, and statistical considerations. Journal of Personality & Social Psychology, 51(6), 1173-1182.
Preacher, K.J., & Hayes, A.F. (2004). SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behavior Research Methods, Instruments, & Computers, 36 (4), 717-731.
Hayes, A. F., & Preacher, K. J. (2010). Quantifying and testing indirect effects in simple mediation models when the constituent paths are nonlinear. Multivariate Behavioral Research, 45(4), 627-660.
This opens the door for the hypothesis that wheat increased mortality in the China Study II sample mainly by displacing dietary fat, and not necessarily by being a primary cause of health problems. In fact, given the strong displacement effect discussed in the previous post, I thought that this hypothesis was quite compelling. I was partly wrong, as you’ll see below.
A counterintuitive hypothesis no doubt, given that wheat is unlikely to have been part of the diet of our Paleolithic ancestors, and thus the modern human digestive tract may be maladapted to it. Moreover, wheat’s main protein (gluten) is implicated in celiac disease, and wheat contains plant toxins such as wheat germ agglutinin.
Still, we cannot completely ignore this hypothesis because: (a) the data points in its general direction; and (b) wheat-based foods are found in way more than trivial amounts in the diets of populations that have relatively high longevity, such as the French.
Testing the hypothesis essentially amounts to testing the significance of two mediating effects; of fat as a mediator of the effects of wheat on mortality, in both the 35-69 and 70-79 age ranges. There are two main approaches for doing this. One is the classic test discussed by Baron & Kenny (1986). The other is the modern test discussed by Preacher & Hayes (2004), and extended by Hayes & Preacher (2010) for nonlinear relationships.
I tested the meditating effects using both approaches, including the nonlinear variation. I used the software WarpPLS for this; the results below are from WarpPLS outputs. Other analyses of the China Study data using WarpPLS can be found here (calorie restriction and longevity), and here (wheat, rice, and cardiovascular disease). For yet other studies, click here.
The graphs below show the path coefficients and chance probabilities of two models. The one at the top-left suggests that wheat flour consumption seems to be associated with a statistically significant increase in mortality in the 70-79 age range (beta=0.23; P=0.04). The effect in the 35-69 age range is almost statistically significant (beta=0.22; P=0.09); the likelihood that it is due to chance is 9 percent (this is the meaning of the P=0.09=9/100=9%).
The graph at the bottom-right suggests that the variable “FatCal”, which is the percentage of calories coming from dietary fat, is indeed a significant mediator of the relationships above between wheat and mortality, in both ranges. But “FatCal” is only a partial mediator.
The reason why “FatCal” is not a “perfect” mediator is that the direct effects of wheat on mortality in both ranges are still relatively strong after “FatCal” is added to the model (i.e., controlled for). In fact, the effects of wheat on mortality don’t change that much with the introduction of the variable “FatCal”.
This analysis suggests that, in the China Study II sample, one of wheat’s main sins might indeed have been to displace dietary fat from animal sources. Wheat consumption is strongly and negatively associated with dietary fat (beta=-0.37; P<0.01), and dietary fat is relatively strongly and negatively associated with mortality in both ranges (more in the 70-79 age range).
Why is dietary fat more protective in the 70-79 than in the 35-69 age range, with the latter effect only being significant at the P=0.10 level (a 10 percent chance probability)? My interpretation is that, as with almost any dietary habit, it takes years for a chronically low fat diet to lead to problems. See graph below; fat was not a huge contributor to the total calorie intake in this sample.
The analysis suggests that wheat also caused problems via other paths. What are them? We can’t say for sure based on this dataset. Perhaps the paths involve lectins and/or gluten. One way or another, the relationship is complex. As you can see from the graph below, the relationship between wheat consumption and mortality is nonlinear for the 70-79 age range, most likely due to confounding factors. The effect size is small for the 35-69 age range, even though it looks linear or quasi-linear in that range.
As you might recall from this post, rice does NOT displace dietary fat, and it seems to be associated with increased longevity. Carbohydrate content per se does not appear to be the problem here. Both rice and wheat foods are rich in them, and have a high glycemic index. Wheat products tend to have a higher glycemic load though.
And why is dietary fat so important as to be significantly associated with increased longevity? This is not a trivial question, because if too much of that fat is stored as body fat it will actually decrease longevity. Dietary fat is very calorie-dense, and can be easily stored as body fat.
Dietary fat is important for various reasons, and probably some that we don’t know about yet. It leads to the formation of body fat, which is not only found in adipocytes or used only as a store of energy. Fat is a key component of a number of important tissues, including 60 percent of our brain. Since fat in the human body undergoes constant turnover, more in some areas than others, lack of dietary fat may compromise the proper functioning of various organs.
Without dietary fat, the very important fat-soluble vitamins (A, D, E and K) cannot be properly absorbed. Taking these vitamins in supplemental form will not work if you don’t consume fat as well. A very low fat diet is almost by definition a diet deficient in fat-soluble vitamins, even if those vitamins are consumed in large amounts via supplements.
Moreover, animals store fat-soluble vitamins in their body fat (as well as in organs), so we get these vitamins in one of their most natural and potent forms when we consume animal fat. Consuming copious amounts of olive and/or coconut oil will not have just the same effect.
References
Baron, R. M., & Kenny, D. A. (1986). The moderator–mediator variable distinction in social psychological research: Conceptual, strategic, and statistical considerations. Journal of Personality & Social Psychology, 51(6), 1173-1182.
Preacher, K.J., & Hayes, A.F. (2004). SPSS and SAS procedures for estimating indirect effects in simple mediation models. Behavior Research Methods, Instruments, & Computers, 36 (4), 717-731.
Hayes, A. F., & Preacher, K. J. (2010). Quantifying and testing indirect effects in simple mediation models when the constituent paths are nonlinear. Multivariate Behavioral Research, 45(4), 627-660.
Sunday, February 13, 2011
Does protein leach calcium from the bones? Yes, but only if it is plant protein
The idea that protein leaches calcium from the bones has been around for a while. It is related to the notion that protein, especially from animal foods, increases blood acidity. The body then uses its main reservoir of calcium, the bones, to reduce blood acidity. Chris Masterjohn does not agree with this idea. This post generally supports Chris’s view, and adds a twist to it, related to plant protein consumption.
The “eat-meat-lose-bone” idea has apparently become popular due to the position taken by Loren Cordain on the topic. Dr. Cordain has also made several important and invaluable contributions to our understanding of the diets of our Paleolithic ancestors. He has argued in his book, The Paleo Diet, and elsewhere (see, e.g., here) that to counter the acid load of protein one should eat fruits and vegetables. The latter are believed to have an alkaline load.
If the idea that protein leaches calcium from the bones is correct, one would expect to see a negative association between protein consumption and bone mineral density (BMD). This negative association should be particularly strong in people aged 50 and older, who are more vulnerable to BMD losses.
As it turns out, this idea appears to be correct only for plant protein. Animal protein seems to be associated with an increase in BMD, at least according to a study by Promislow et al. (2002). The study shows that there is a positive multivariate association between animal protein consumption and BMD; an association that becomes negative when plant protein consumption is considered.
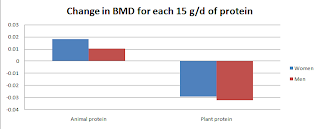
The study focused on 572 women and 388 men aged 55–92 years living in Rancho Bernardo, California. Food frequency questionnaires were administered in the 1988–1992 period, and BMD was measured 4 years later. The bar chart below shows the approximate increases in BMD (in g/cm^2) for each 15 g/d increment in protein intake.
The authors reported increments in BMD for different increments of protein (15 and 5 g/d), so the results above are adjusted somewhat from the original values reported in the article. Keeping that in mind, the increment in BMD for men due to animal protein was not statistically significant (P=0.20). That is the smallest bar on the left.
Does protein leach calcium from the bones? Based on this study, the reasonable answers to this question are yes for plant protein, and no for animal protein. For animal protein, it seems to be quite the opposite.
Even more interesting, calcium intake did not seem to be much of a factor. BMD gains due to animal protein seemed to converge to similar values whether calcium intake was high, medium or low. The convergence occurred as animal protein intake increased, and the point of convergence was between 85-90 g/d of animal protein intake.
And high calcium intakes did not seem to protect those whose plant protein consumption was high.
The authors do not discuss specific foods, but one can guess the main plant protein that those folks likely consumed. It was likely gluten from wheat products.
Are the associations above due to: (a) the folks eating animal protein consuming more fruits and vegetables than the folks eating plant protein; or (b) something inherent to animal foods that stimulates an increase in the absorption of dietary calcium, even in small amounts?
This question cannot be answered based on this study; it should have controlled for fruit and vegetable consumption for that.
But if I were to bet, I would bet on (b).
Reference
Promislow, J.H.E., Goodman-Gruen, D., Slymen, D.J., & Barrett-Connor, E. (2002). Protein consumption and bone mineral density in the elderly. American Journal of Epidemiology, 155(7), 636–644.
The “eat-meat-lose-bone” idea has apparently become popular due to the position taken by Loren Cordain on the topic. Dr. Cordain has also made several important and invaluable contributions to our understanding of the diets of our Paleolithic ancestors. He has argued in his book, The Paleo Diet, and elsewhere (see, e.g., here) that to counter the acid load of protein one should eat fruits and vegetables. The latter are believed to have an alkaline load.
If the idea that protein leaches calcium from the bones is correct, one would expect to see a negative association between protein consumption and bone mineral density (BMD). This negative association should be particularly strong in people aged 50 and older, who are more vulnerable to BMD losses.
As it turns out, this idea appears to be correct only for plant protein. Animal protein seems to be associated with an increase in BMD, at least according to a study by Promislow et al. (2002). The study shows that there is a positive multivariate association between animal protein consumption and BMD; an association that becomes negative when plant protein consumption is considered.
The study focused on 572 women and 388 men aged 55–92 years living in Rancho Bernardo, California. Food frequency questionnaires were administered in the 1988–1992 period, and BMD was measured 4 years later. The bar chart below shows the approximate increases in BMD (in g/cm^2) for each 15 g/d increment in protein intake.
The authors reported increments in BMD for different increments of protein (15 and 5 g/d), so the results above are adjusted somewhat from the original values reported in the article. Keeping that in mind, the increment in BMD for men due to animal protein was not statistically significant (P=0.20). That is the smallest bar on the left.
Does protein leach calcium from the bones? Based on this study, the reasonable answers to this question are yes for plant protein, and no for animal protein. For animal protein, it seems to be quite the opposite.
Even more interesting, calcium intake did not seem to be much of a factor. BMD gains due to animal protein seemed to converge to similar values whether calcium intake was high, medium or low. The convergence occurred as animal protein intake increased, and the point of convergence was between 85-90 g/d of animal protein intake.
And high calcium intakes did not seem to protect those whose plant protein consumption was high.
The authors do not discuss specific foods, but one can guess the main plant protein that those folks likely consumed. It was likely gluten from wheat products.
Are the associations above due to: (a) the folks eating animal protein consuming more fruits and vegetables than the folks eating plant protein; or (b) something inherent to animal foods that stimulates an increase in the absorption of dietary calcium, even in small amounts?
This question cannot be answered based on this study; it should have controlled for fruit and vegetable consumption for that.
But if I were to bet, I would bet on (b).
Reference
Promislow, J.H.E., Goodman-Gruen, D., Slymen, D.J., & Barrett-Connor, E. (2002). Protein consumption and bone mineral density in the elderly. American Journal of Epidemiology, 155(7), 636–644.
Labels:
blood acidity,
bone density,
calcium,
protein,
research
Polyphenols, Hormesis and Disease: Part I
What are Polyphenols?
Polyphenols are a diverse class of molecules containing multiple phenol rings. They are synthesized in large amounts by plants, certain fungi and a few animals, and serve many purposes, including defense against predators/infections, defense against sunlight damage and chemical oxidation, and coloration. The color of many fruits and vegetables, such as blueberries, eggplants, red potatoes and apples comes from polyphenols. Some familiar classes of polyphenols in the diet-health literature are flavonoids, isoflavonoids, anthocyanidins, and lignins.
The Case Against Polyphenols
Many diet-health authorities seem pretty well convinced that dietary polyphenols are an important part of good health, due to their supposed antioxidant properties. In the past, I've been critical of the hypothesis. There are several reasons for it:
A Reappraisal
After reading more about polyphenols, and coming to understand that the prevailing hypothesis of why they work makes no sense, I decided that the whole thing is probably bunk: at best, specific polyphenols are protective in rodents at unnaturally high doses due to some drug-like effect. But-- I kept my finger on the pulse of the field just in case, and I began to notice that more sophisticated studies were emerging almost weekly that seemed to confirm that realistic amounts of certain polyphenol-rich foods (not just massive quantities of polyphenol extract) have protective effects against a variety of health problems. There are many such studies, and I won't attempt to review them comprehensively, but here are a few I've come across:
In the face of this accumulating evidence, I've had to reconsider my position on polyphenols. In the process, and through conversations with knowledgeable researchers in the polyphenol field, I encountered a different hypothesis that puts the puzzle pieces together nicely. I'll discuss that in the next post.
* Serum levels of polyphenols briefly enter the mid nM to low uM range, depending on the food (2). Compare that with the main serum antioxidants: ~200 uM for uric acid, ~100 uM for vitamin C, ~30 uM for vitamin E.
Polyphenols are a diverse class of molecules containing multiple phenol rings. They are synthesized in large amounts by plants, certain fungi and a few animals, and serve many purposes, including defense against predators/infections, defense against sunlight damage and chemical oxidation, and coloration. The color of many fruits and vegetables, such as blueberries, eggplants, red potatoes and apples comes from polyphenols. Some familiar classes of polyphenols in the diet-health literature are flavonoids, isoflavonoids, anthocyanidins, and lignins.
The Case Against Polyphenols
Many diet-health authorities seem pretty well convinced that dietary polyphenols are an important part of good health, due to their supposed antioxidant properties. In the past, I've been critical of the hypothesis. There are several reasons for it:
- Polyphenols are often, but not always, defensive compounds that interfere with digestive processes, which is why they often taste bitter and/or astringent. Plant-eating animals including humans have evolved defensive strategies against polyphenol-rich foods, such as polyphenol-binding proteins in saliva (1).
- Ingested polyphenols are poorly absorbed (2). The concentration in blood is low, and the concentration inside cells is probably considerably lower*. In contrast, essential antioxidant nutrients such as vitamins E and C are efficiently absorbed and retained rather than excluded from the circulation.
- Polyphenols that manage to cross the gut barrier are rapidly degraded by the liver, just like a variety of other foreign molecules, again suggesting that the body doesn't want them hanging around (2).
- The most visible hypothesis of how polyphenols influence health is the idea that they are antioxidants, protecting against the ravages of reactive oxygen species. While many polyphenols are effective antioxidants at high concentrations in a test tube, I don't find it very plausible that the low and transient blood concentration of polyphenols achieved by eating polyphenol-rich foods makes a meaningful contribution to that person's overall antioxidant status, when compared to the relatively high concentrations of other antioxidants in blood* (uric acid; vitamins C, E; ubiquinone) and particularly inside cells (SOD1/2, catalase, glutathione reductase, thioredoxin reductase, paraoxonase 1, etc.).
- There are a number of studies showing that the antioxidant capacity of the blood increases after eating polyphenol-rich foods. These are often confounded by the fact that fructose (in fruit and some vegetables) and caffeine (in tea and coffee) can increase the blood level of uric acid, the blood's main water-soluble antioxidant. Drinking sugar water has the same effect (2).
- Rodent studies showing that polyphenols improve health typically use massive doses that exceed what a person could consume eating food, and do not account for the possibility that the rodents may have been calorie restricted because their food tastes awful.
A Reappraisal
After reading more about polyphenols, and coming to understand that the prevailing hypothesis of why they work makes no sense, I decided that the whole thing is probably bunk: at best, specific polyphenols are protective in rodents at unnaturally high doses due to some drug-like effect. But-- I kept my finger on the pulse of the field just in case, and I began to notice that more sophisticated studies were emerging almost weekly that seemed to confirm that realistic amounts of certain polyphenol-rich foods (not just massive quantities of polyphenol extract) have protective effects against a variety of health problems. There are many such studies, and I won't attempt to review them comprehensively, but here are a few I've come across:
- Dr. David Grassi and colleagues showed that polyphenol-rich chocolate lowers blood pressure, improves insulin sensitivity and lowers LDL cholesterol in hypertensive and insulin resistant volunteers when compared with white chocolate (3). Although dark chocolate is also probably richer in magnesium, copper and other nutrients than white chocolate, the study is still intriguing.
- Dr. Christine Morand and colleagues showed that drinking orange juice every day lowers blood pressure and increases vascular reactivity in overweight volunteers, an effect that they were able to specifically attribute to the polyphenol hesperidin (4).
- Dr. F. Natella and colleagues showed that red wine prevents the increase in oxidized blood lipids (fats) that occurs after consuming a meal high in oxidized and potentially oxidizable fats (5).
- Several studies have shown that hibiscus tea lowers blood pressure in people with hypertension when consumed regularly (6, 7, 8). It also happens to be delicious.
- Dr. Arpita Basu and colleagues showed that blueberries lower blood pressure and oxidized LDL in men and women with metabolic syndrome (9).
- Animal studies have generally shown similar results. Dr. Xianli Wu and colleagues showed that whole blueberries potently inhibit atherosclerosis (hardening and thickening of the arteries that can lead to a heart attack) in a susceptible strain of mice (10). This effect was associated with a higher expression level of antioxidant enzymes in the vessel walls and other tissues.
In the face of this accumulating evidence, I've had to reconsider my position on polyphenols. In the process, and through conversations with knowledgeable researchers in the polyphenol field, I encountered a different hypothesis that puts the puzzle pieces together nicely. I'll discuss that in the next post.
* Serum levels of polyphenols briefly enter the mid nM to low uM range, depending on the food (2). Compare that with the main serum antioxidants: ~200 uM for uric acid, ~100 uM for vitamin C, ~30 uM for vitamin E.
Thursday, February 10, 2011
My Gluten-Free January
I've been avoiding most gluten, particularly wheat, for over a year now. I never had obvious symptoms that I could clearly link to eating wheat, although I had my suspicions. I've made many changes to my diet over the last decade, and I feel much better than I did ten years ago, but it's hard to disentangle all the factors. I don't think I ever went an entire month without eating any gluten at all before this January. After posting Matt Lentzner's challenge to go gluten-free this January, I felt obligated to do it myself, so I signed up!
I succeeded in avoiding all gluten for the month of January, even though it was a pain at times. I felt good before January, and didn't start with any health or body weight problems, so there wasn't much to improve. I also felt good while strictly avoiding gluten this January, perhaps a little better than usual but it's hard to say.
At the end of the month, I did a blinded wheat challenge using the method I described in a previous post, which uses gluten-free bread as the placebo (1). I recorded my blood sugar at 30 minute intervals after eating the bread, and recorded how I felt physically and emotionally for three days after each challenge.
The result? I think the bread gave me gas, but that's about it. I'm not even positive that was due to the wheat. My energy level was good, and I didn't experience any digestive pain or changes in transit time. There was no significant difference in my blood glucose response between the bread and the gluten-free bread.
I decided that I didn't have any symptoms, so I celebrated by having a porter (1) with friends a few nights later. I slept poorly and woke up with mild digestive discomfort and gas. Then I ate wheat later in the week and slept poorly and got gas again. Hmmm...
Some people might say that the body adapts to any food, and wheat is no different. Go without it for a while, and the body has a tough time digesting it. But I can go for weeks without eating a potato, a chicken thigh or broccoli, and all will digest just fine when I eat them again.
I'm pretty sure I don't have a severe reaction to gluten. I think I'm going to stick with my mostly gluten-free habits, and eat it occasionally when I'm offered food in social situations.
Did anyone else do a blinded wheat challenge? Describe it in the comments!
I succeeded in avoiding all gluten for the month of January, even though it was a pain at times. I felt good before January, and didn't start with any health or body weight problems, so there wasn't much to improve. I also felt good while strictly avoiding gluten this January, perhaps a little better than usual but it's hard to say.
At the end of the month, I did a blinded wheat challenge using the method I described in a previous post, which uses gluten-free bread as the placebo (1). I recorded my blood sugar at 30 minute intervals after eating the bread, and recorded how I felt physically and emotionally for three days after each challenge.
The result? I think the bread gave me gas, but that's about it. I'm not even positive that was due to the wheat. My energy level was good, and I didn't experience any digestive pain or changes in transit time. There was no significant difference in my blood glucose response between the bread and the gluten-free bread.
I decided that I didn't have any symptoms, so I celebrated by having a porter (1) with friends a few nights later. I slept poorly and woke up with mild digestive discomfort and gas. Then I ate wheat later in the week and slept poorly and got gas again. Hmmm...
Some people might say that the body adapts to any food, and wheat is no different. Go without it for a while, and the body has a tough time digesting it. But I can go for weeks without eating a potato, a chicken thigh or broccoli, and all will digest just fine when I eat them again.
I'm pretty sure I don't have a severe reaction to gluten. I think I'm going to stick with my mostly gluten-free habits, and eat it occasionally when I'm offered food in social situations.
Did anyone else do a blinded wheat challenge? Describe it in the comments!
Wednesday, February 9, 2011
Gluten-Free January Raffle!
Hi, Gluten-Free January participants. Matt, Janine and I have collected about 200 survey responses at this point. So far, the results are very interesting! But we want to get as many responses as possible, because the more responses we get, the more informative the data will be for all of us. So please fill out the survey Matt sent you by e-mail, no matter what your results were, and no matter whether you stuck with the diet or not! The survey is strictly about your GFJ experience, not investment opportunities, timeshares, ShamWows or anything else. It will take you less than 5 minutes, and it's totally anonymous. The deadline is Feb 15th. Big thanks to everyone who has taken it so far.
To encourage participants to complete the survey, we're organizing a raffle. Matt and I have five Gluten-Free January T-shirts we're ready to give out for free. These shirts were designed by Matt and they're really cool. I have one myself, and the print and fabric quality are top notch. Here's what the logo looks like:
 If you've completed the survey and want to be included in the raffle, please e-mail Matt to let him know you've completed it. Anyone who has already e-mailed Matt to let him know they completed the survey will automatically be entered, so no need for a second e-mail. So far, very few people have written Matt, so your probability of winning a shirt is high!
If you've completed the survey and want to be included in the raffle, please e-mail Matt to let him know you've completed it. Anyone who has already e-mailed Matt to let him know they completed the survey will automatically be entered, so no need for a second e-mail. So far, very few people have written Matt, so your probability of winning a shirt is high!
To encourage participants to complete the survey, we're organizing a raffle. Matt and I have five Gluten-Free January T-shirts we're ready to give out for free. These shirts were designed by Matt and they're really cool. I have one myself, and the print and fabric quality are top notch. Here's what the logo looks like:
 If you've completed the survey and want to be included in the raffle, please e-mail Matt to let him know you've completed it. Anyone who has already e-mailed Matt to let him know they completed the survey will automatically be entered, so no need for a second e-mail. So far, very few people have written Matt, so your probability of winning a shirt is high!
If you've completed the survey and want to be included in the raffle, please e-mail Matt to let him know you've completed it. Anyone who has already e-mailed Matt to let him know they completed the survey will automatically be entered, so no need for a second e-mail. So far, very few people have written Matt, so your probability of winning a shirt is high!Sunday, February 6, 2011
Is working standing up too expensive? It could cost you as little as $10
Spending too much time sitting down is clearly unnatural, particularly if you sit down on very comfortable chairs. Sitting down per se is probably natural, given the human anatomy, but not sitting down for hours in the same position. Also, comfortable furniture is an apparently benign Neolithic invention, but over several years it may stealthily contributed to the metabolic syndrome and the diseases of civilization.
Getting an elevated workstation may be a bit expensive. At work, you may have to go through a bit of a battle with your employer to get it (unless you are "teh boz"), only to find out that having to work standing up all the time is not what you really wanted. That may not be very natural either. So what is one to do? One possible solution is to buy a small foldable plastic table (or chair) like the one on the figure below, which may cost you less than $10, and put it on your work desk. I have been doing this for quite a while now, and it works fine for me.
The photo above shows a laptop computer. Nevertheless, you can use this table-over-table approach with a desktop computer as well. And you still keep the space under the foldable table, which you can use to place other items. With a desktop computer this approach would probably require two foldable tables to elevate the screen, keyboard, and mouse. This approach also works for reading documents and writing with a pen or pencil; just put a thick sheet of paper on the foldable table to make a flat surface (if the foldable table’s surface is not flat already). And you don’t have to be standing up all the time; you can sit down as well after removing the foldable table. It takes me about 5 seconds to do or undo this setup.
When you sit down, you may want to consider using a pillow like the one on the photo to force yourself to sit upright. (You can use it as shown, or place the pillow flat on the chair and sit on its edge.) Sitting on a very comfy chair with back support prevents you from using the various abdominal and back muscles needed to maintain posture. As a result, you may find yourself unusually prone to low back injuries and suffering from “mysterious” abdominal discomfort. You will also very likely decrease your nonexercise activity thermogenesis (NEAT), which is a major calorie expenditure regulator.
With posture stabilization muscles, as with almost everything else in the human body, the reality is this: if you don’t use them, you lose them.
Getting an elevated workstation may be a bit expensive. At work, you may have to go through a bit of a battle with your employer to get it (unless you are "teh boz"), only to find out that having to work standing up all the time is not what you really wanted. That may not be very natural either. So what is one to do? One possible solution is to buy a small foldable plastic table (or chair) like the one on the figure below, which may cost you less than $10, and put it on your work desk. I have been doing this for quite a while now, and it works fine for me.
The photo above shows a laptop computer. Nevertheless, you can use this table-over-table approach with a desktop computer as well. And you still keep the space under the foldable table, which you can use to place other items. With a desktop computer this approach would probably require two foldable tables to elevate the screen, keyboard, and mouse. This approach also works for reading documents and writing with a pen or pencil; just put a thick sheet of paper on the foldable table to make a flat surface (if the foldable table’s surface is not flat already). And you don’t have to be standing up all the time; you can sit down as well after removing the foldable table. It takes me about 5 seconds to do or undo this setup.
When you sit down, you may want to consider using a pillow like the one on the photo to force yourself to sit upright. (You can use it as shown, or place the pillow flat on the chair and sit on its edge.) Sitting on a very comfy chair with back support prevents you from using the various abdominal and back muscles needed to maintain posture. As a result, you may find yourself unusually prone to low back injuries and suffering from “mysterious” abdominal discomfort. You will also very likely decrease your nonexercise activity thermogenesis (NEAT), which is a major calorie expenditure regulator.
With posture stabilization muscles, as with almost everything else in the human body, the reality is this: if you don’t use them, you lose them.
Saturday, February 5, 2011
Assorted Thoughts About the 2010 Dietary Guidelines
In the past week, I've been rooting through the USDA's 2010 Dietary Guidelines (1). Here are a few of my thoughts.
Positive
One of the things I've been enjoying recently is watching health authorities shift away from a nutrient-oriented philosophy in favor of a more food-oriented philosophy. For example, I recently read a nice editorial by Drs. Dariush Mozaffarian and David S. Ludwig (not associated with the USDA) that encapsulates this (2). Here's a quote:
Although the 2010 guidelines are too focused on nutrients for my taste, they do spend some time talking about food groups and eating patterns, for example, recommending an increase in the consumption of vegetables, fruit, whole grains and seafood. They also recommend Mediterranean and plant-focused eating patterns. Although I don't think their recommendations quite hit the mark, they do reflect a shift in thinking.
Another thing I enjoyed about the Guidelines is the table on page 12 of chapter 2, which shows just how messed up the average American diet is. The number one source of calories in all age groups is "grain-based desserts". The next five in adults are yeast breads, chicken dishes, soda/sports drinks, alcohol and pizza. To see typical American food habits presented like this just blows me away. They call this the "obesogenic environment"; the idea that we're surrounded by tasty but unhealthy food and situations that favor the consumption of it. I agree.
The Guidelines also contain a surprisingly accurate one-sentence review of the glycemic index literature:
The first problem is the creation of the category "solid fats and added sugars", abbreviated SoFAS. With the creation of this term, they lump pastured butter together with Crisco and Red Hots. If they've been hiding the evidence that pastured butter, virgin coconut oil or red palm oil contribute to heart disease, I'd like to see it so I can stop eating them!
Another problem is their list of recommendations to curb the obesity epidemic. They say:
Jokes aside, I do think energy balance is a huge issue, perhaps even the central issue in chronic disease risk in affluent nations. The basic problem is that Americans are eating more calories than is optimal, and they have a very hard time stopping. It's not because they have less willpower than their stoic ancestors, it's because their bodies have decided that overweight/obesity is the new lean, and they defend that higher level of fat mass against changes. Simply telling an overweight person to eat fewer calories, without changing the dietary context, is not very effective in the long term, due to compensatory mechanisms including hunger and increased metabolic efficiency (fewer calories burned for the same muscular exertion).
What does the USDA recommend to lose fat or maintain leanness?
At one point, they talk about changes in the US diet that have corresponded with the obesity epidemic:
Conclusion
Although the 2010 USDA Dietary Guidelines show some promising trends, and contain some good information, I hope you can find a better source than the USDA for your nutrition advice.
Positive
One of the things I've been enjoying recently is watching health authorities shift away from a nutrient-oriented philosophy in favor of a more food-oriented philosophy. For example, I recently read a nice editorial by Drs. Dariush Mozaffarian and David S. Ludwig (not associated with the USDA) that encapsulates this (2). Here's a quote:
Nutritional science has advanced rapidly, and the evidence now demonstrates the major limitations of nutrient-based metrics for prevention of chronic disease. The proportion of total energy from fat appears largely unrelated to risk of cardiovascular disease, cancer, diabetes, or obesity. Saturated fat—targeted by nearly all nutrition-related professional organizations and governmental agencies—has little relation to heart disease within most prevailing dietary patterns. Typical recommendations to consume at least half of total energy as carbohydrate, a nutrient for which humans have no absolute requirement, conflate foods with widely divergent physiologic effects (eg, brown rice, white bread, apples). Foods are grouped based on protein content (chicken, fish, beans, nuts) despite demonstrably different health effects. With few exceptions (eg, omega-3 fats, trans fat, salt), individual compounds in isolation have small effects on chronic diseases. Thus, little of the information found on food labels’ “nutrition facts” panels provides useful guidance for selecting healthier foods to prevent chronic disease.Tell it! Although he doesn't use the word nutritionism, that's basically what he's arguing against. Dr. Mozaffarian seems to represent the less reductionist school of nutrition, which is a more informed version of what nutrition pioneers such as Sir Edward Mellanby, Dr. May Mellanby, Dr. Weston Price and Sir Robert McCarrison advocated.
In contrast with discrete nutrients, specific foods and dietary patterns substantially affect chronic disease risk, as shown by controlled trials of risk factors and prospective cohorts of disease end points
Although this approach may seem radical, it actually represents a return to more traditional, time-tested ways of eating. Healthier food-based dietary patterns have existed for generations among some populations.
Although the 2010 guidelines are too focused on nutrients for my taste, they do spend some time talking about food groups and eating patterns, for example, recommending an increase in the consumption of vegetables, fruit, whole grains and seafood. They also recommend Mediterranean and plant-focused eating patterns. Although I don't think their recommendations quite hit the mark, they do reflect a shift in thinking.
Another thing I enjoyed about the Guidelines is the table on page 12 of chapter 2, which shows just how messed up the average American diet is. The number one source of calories in all age groups is "grain-based desserts". The next five in adults are yeast breads, chicken dishes, soda/sports drinks, alcohol and pizza. To see typical American food habits presented like this just blows me away. They call this the "obesogenic environment"; the idea that we're surrounded by tasty but unhealthy food and situations that favor the consumption of it. I agree.
The Guidelines also contain a surprisingly accurate one-sentence review of the glycemic index literature:
Strong evidence shows that glycemic index and/or glycemic load are not associated with body weight; thus, it is not necessary to consider these measures when selecting carbohydrate foods and beverages for weight management.Negative
The first problem is the creation of the category "solid fats and added sugars", abbreviated SoFAS. With the creation of this term, they lump pastured butter together with Crisco and Red Hots. If they've been hiding the evidence that pastured butter, virgin coconut oil or red palm oil contribute to heart disease, I'd like to see it so I can stop eating them!
Another problem is their list of recommendations to curb the obesity epidemic. They say:
The current high rates of overweight and obesity among virtually all subgroups of the population in the United States demonstrate that many Americans are in calorie imbalance—that is, they consume more calories than they expend. To curb the obesity epidemic and improve their health, Americans need to make significant efforts to decrease the total number of calories they consume from foods and beverages and increase calorie expenditure through physical activity.Looks like we have Sherlock Holmes on the case. Now that we have this information, all we have to do is tell overweight people to eat less and they'll be lean again! What's that, they already know and it's not working?? Someone should tell the USDA.
Jokes aside, I do think energy balance is a huge issue, perhaps even the central issue in chronic disease risk in affluent nations. The basic problem is that Americans are eating more calories than is optimal, and they have a very hard time stopping. It's not because they have less willpower than their stoic ancestors, it's because their bodies have decided that overweight/obesity is the new lean, and they defend that higher level of fat mass against changes. Simply telling an overweight person to eat fewer calories, without changing the dietary context, is not very effective in the long term, due to compensatory mechanisms including hunger and increased metabolic efficiency (fewer calories burned for the same muscular exertion).
What does the USDA recommend to lose fat or maintain leanness?
- Count calories. Doesn't work for most people, although I acknowledge that it is physically possible to lose fat (and lean mass) by restricting calories.
- Reduce sweetened beverages. Thumbs up.
- Serve smaller portions. As far as I know, this rests exclusively on very short-term studies that showed that food consumed at a single meal or three is reduced if portion size is smaller. I guess it can't hurt to try it, but I'm not convinced it will have any effect on long-term body fatness. I think restaurant portion sizes have probably increased because people eat more, rather than the other way around, although both could be true.
- Eat foods that are less calorie dense. I think vegetables are healthy, but is it because they're less calorie-dense? Why is dietary fat intake generally not associated with obesity if it's the most calorie-dense substance? Why do many people lose body fat eating energy-dense low-carbohydrate diets? Not convinced, but I'm feeling open minded about this one.
- Exercise more and watch less TV. Exercise is good. But don't let it make you hungry, because then you'll eat more!
At one point, they talk about changes in the US diet that have corresponded with the obesity epidemic:
Average daily calories available per person in the marketplace increased approximately 600 calories, with the greatest increases in the availability of added fats and oils, grains, milk and milk products, and caloric sweeteners.Let me edit that so it's more complete:
Average daily calories available per person in the marketplace increased approximately 600 calories per day, 250 calories of which were actually consumed (USDA and NHANES). Added fats increased, due to a large increase in seed oil intake, but total fat intake remained approximately the same because of a roughly equal decrease in fatty meat and whole milk consumption (USDA and NHANES). Grain intake, predominantly wheat, increased, as did the consumption of refined sweeteners, predominantly high-fructose corn syrup (USDA).It reads a bit differently once you have a little more information, doesn't it? Animal fat intake declined considerably, and was replaced by seed oils, in parallel with the obesity and diabetes epidemics. Maybe it contributed, maybe it didn't, but why not just be forthright about it? People appreciate honesty.
Conclusion
Although the 2010 USDA Dietary Guidelines show some promising trends, and contain some good information, I hope you can find a better source than the USDA for your nutrition advice.
Labels:
diet,
overweight
Subscribe to:
Posts (Atom)