Filet mignon is one of the tenderest cuts of beef. It is also one of my favorites. Filet mignon comes from the tenderloin area (see this picture), which is not a weight-bearing area and thus is very tender. The bison cuts I get here in South Texas are close in terms of tenderness, but not as tender, probably because they are from the round area.
One steak of either filet mignon or bison will yield about 100 g of cooked meat, with 30 g of protein and 10 g of fat. About half of that fat will be saturated and half monounsaturated (as in olive oil). It will provide you with plenty of vitamins (particular B vitamins) and minerals. Good amounts of selenium, phosphorus, zinc and potassium.
On the photo below (click on it to enlarge), the bison steak is at the top. The other pieces are all filet mignon cuts. They are all medium-cooked. I cooked two plates of these, for 6 people. All ate to satisfaction, with a side salad. The leftovers are delicious for breakfast in small amounts.
For the filet mignon, I think you really have to go to a specialty meats store (butcher) and make sure that they cut the smaller tail end of the tenderloin muscle. You will be paying a lot for it, so it makes sense to be choosy. Experience butchers will cut it right in front of you and won’t mind your choosiness.
Below is a simple recipe; simple like most of the recipes on this blog. I like my meals quick and delicious.
- Prepare some dry seasoning powder by mixing sea salt, garlic power, chili powder, and a small amount of cayenne pepper.
- Season the steaks at least 2 hours prior to placing them on the grill.
- Grill with the lid on, checking the meat every 10 minutes or so. (I use charcoal, one layer only to avoid burning the surface of the meat.) Turn it frequently, always putting the lid back on.
- If you like it rare, 20 minutes (or a bit less) may be enough.
These are as tender as any piece of beef can possibly get. No need for any tenderizer juices during seasoning. If you are doing both filet mignon and bison together, either eat only bison or bison first. Because once you taste the filet mignon, the bison cut may taste a bit hard!
For me the filet mignon is a 10-dollar per pound treat for special occasions. The price of the bison cut is about the same, at least here in Laredo, Texas, where I get it shipped from Dakota via my local supermarket. You can also get it online.
By the way, some folks like to say that bison is the “salmon of the prairie”. This is in reference to bison’s omega-3 content. Well, here is the polyunsaturated fatty acid composition of 100 g of bison steak: 29 mg of omega-3, and 197 mg of omega-6. For salmon it is 1424 mg of omega-3, and 113 mg of omega-6.
Salmon of the prairie or not, I love it!
Thursday, April 29, 2010
Wednesday, April 28, 2010
Grains as Food: an Update
Improperly Prepared Grain Fiber can be Harmful
Last year, I published a post on the Diet and Reinfarction trial (DART), a controlled trial that increased grain fiber intake using whole wheat bread and wheat bran supplements, and reported long-term health outcomes in people who had previously suffered a heart attack (1). The initial paper found a trend toward increased heart attacks and deaths in the grain fiber-supplemented group at two years, which was not statistically significant.
What I didn't know at the time is that a follow-up study has been published. After mathematically "adjusting" for preexisting conditions and medication use, the result reached statistical significance: people who increased their grain fiber intake had more heart attacks than people who didn't during the two years of the controlled trial. Overall mortality was higher as well, but that didn't reach statistical significance. You have to get past the abstract of the paper to realize this, but fortunately it's free access (2).
Here's a description of what not to eat if you're a Westerner with established heart disease:
The term 'fiber' can refer to many different things. Dietary fiber is simply defined as an edible substance that doesn't get digested by the human body. It doesn't even necessarily come from plants. If you eat a shrimp with the shell on, and the shell comes out the other end (which it will), it was fiber.
Grain fiber is a particular class of dietary fiber that has specific characteristics. It's mostly cellulose (like wood; although some grains are rich in soluble fiber as well), and it contains a number of defensive substances and storage molecules that make it more difficult to eat. These may include phytic acid, protease inhibitors, amylase inhibitors, lectins, tannins, saponins, and goitrogens (3). Grain fiber is also a rich source of vitamins and minerals, although the minerals are mostly inaccessible due to grains' high phytic acid content (4, 5, 6).
Every plant food (and some animal foods) has its chemical defense strategy, and grains are no different*. It's just that grains are particularly good at it, and also happen to be one of our staple foods in the modern world. If you don't think grains are naturally inedible for humans, try eating a heaping bowl full of dry, raw whole wheat berries.
Human Ingenuity to the Rescue
Humans are clever creatures, and we've found ways to use grains as a food source, despite not being naturally adapted to eating them**. The most important is our ability to cook. Cooking deactivates many of the harmful substances found in grains and other plant foods. However, some are not deactivated by cooking. These require other strategies to remove or deactivate.
Healthy grain-based cultures don't prepare their grains haphazardly. Throughout the world, using a number of different grains, many have arrived at similar strategies for making grains edible and nutritious. The most common approach involves most or all of these steps:
In the next post, I'll explain why these processing steps greatly improve the nutritional value of grains, and I'll describe recipes from around the world to illustrate the point.
* Including tubers. For example, sweet potatoes contain goitrogens, oxalic acid, and protease inhibitors. Potatoes contain toxic glycoalkaloids. Taro contains oxalic acid and protease inhibitors. Cassava contains highly toxic cyanogens. Some of these substances are deactivated by cooking, others are not. Each food has an associated preparation method that minimizes its toxic qualities. Potatoes are peeled, removing the majority of the glycoalkaloids. Cassava is grated and dried or fermented to inactivate cyanogens. Some cultures ferment taro.
** As opposed to mice, for example, which can survive on raw whole grains.
Last year, I published a post on the Diet and Reinfarction trial (DART), a controlled trial that increased grain fiber intake using whole wheat bread and wheat bran supplements, and reported long-term health outcomes in people who had previously suffered a heart attack (1). The initial paper found a trend toward increased heart attacks and deaths in the grain fiber-supplemented group at two years, which was not statistically significant.
What I didn't know at the time is that a follow-up study has been published. After mathematically "adjusting" for preexisting conditions and medication use, the result reached statistical significance: people who increased their grain fiber intake had more heart attacks than people who didn't during the two years of the controlled trial. Overall mortality was higher as well, but that didn't reach statistical significance. You have to get past the abstract of the paper to realize this, but fortunately it's free access (2).
Here's a description of what not to eat if you're a Westerner with established heart disease:
Those randomised to fibre advice were encouraged to eat at least six slices of wholemeal bread per day, or an equivalent amount of cereal fibre from a mixture of wholemeal bread, high-fibre breakfast cereals and wheat bran.Characteristics of Grain Fiber
The term 'fiber' can refer to many different things. Dietary fiber is simply defined as an edible substance that doesn't get digested by the human body. It doesn't even necessarily come from plants. If you eat a shrimp with the shell on, and the shell comes out the other end (which it will), it was fiber.
Grain fiber is a particular class of dietary fiber that has specific characteristics. It's mostly cellulose (like wood; although some grains are rich in soluble fiber as well), and it contains a number of defensive substances and storage molecules that make it more difficult to eat. These may include phytic acid, protease inhibitors, amylase inhibitors, lectins, tannins, saponins, and goitrogens (3). Grain fiber is also a rich source of vitamins and minerals, although the minerals are mostly inaccessible due to grains' high phytic acid content (4, 5, 6).
Every plant food (and some animal foods) has its chemical defense strategy, and grains are no different*. It's just that grains are particularly good at it, and also happen to be one of our staple foods in the modern world. If you don't think grains are naturally inedible for humans, try eating a heaping bowl full of dry, raw whole wheat berries.
Human Ingenuity to the Rescue
Humans are clever creatures, and we've found ways to use grains as a food source, despite not being naturally adapted to eating them**. The most important is our ability to cook. Cooking deactivates many of the harmful substances found in grains and other plant foods. However, some are not deactivated by cooking. These require other strategies to remove or deactivate.
Healthy grain-based cultures don't prepare their grains haphazardly. Throughout the world, using a number of different grains, many have arrived at similar strategies for making grains edible and nutritious. The most common approach involves most or all of these steps:
- Soaking
- Grinding
- Removing 50-75% of the bran
- Sour fermentation
- Cooking
In the next post, I'll explain why these processing steps greatly improve the nutritional value of grains, and I'll describe recipes from around the world to illustrate the point.
* Including tubers. For example, sweet potatoes contain goitrogens, oxalic acid, and protease inhibitors. Potatoes contain toxic glycoalkaloids. Taro contains oxalic acid and protease inhibitors. Cassava contains highly toxic cyanogens. Some of these substances are deactivated by cooking, others are not. Each food has an associated preparation method that minimizes its toxic qualities. Potatoes are peeled, removing the majority of the glycoalkaloids. Cassava is grated and dried or fermented to inactivate cyanogens. Some cultures ferment taro.
** As opposed to mice, for example, which can survive on raw whole grains.
Friday, April 23, 2010
There are more geniuses among men than among women, and more idiots too
Deary and colleagues (2007) conducted an interesting study on differences in intelligence scores among men and women. In the context of this blog, this study highlights yet one more counterintuitive and intriguing aspect of Darwinian evolution, adding to points previously made in other posts (see here, and here). Evolution may look simple at first glance, but that is a bit of a mirage. In my opinion, to really understand it one has to understand the mathematics underlying it, a lot of which comes from the field of population genetics.
What makes the study by Deary and colleagues (2007) particularly interesting is that its participants were opposite-sex siblings. This helped control for the influence of environmental factors. The downside is that the effect sizes might have been decreased, because of the high gene correlation among siblings, so we could expect larger differences between unrelated groups of men women. The differences, as you will see, are not in overall scores, but in score dispersion.
Let us get straight to the point made by the study. On average, men and women seem to score equally well on intelligence tests. The main difference is that there is more variation in the scores achieved by men than by women, which leads to an interesting effect: there are more geniuses and more idiots among men than among women.
This does NOT mean that a man’s genius is of a higher order; just that there is a tendency for more men to be geniuses (and idiots) than women in any random population sample. The women who are geniuses can be super geniuses, like two-time Nobel Prize winner Marie Curie, the first PERSON to receive such an honor. Albert Einstein is said that have greatly admired her intelligence.
As an illustration of this score dispersion effect, Deary and colleagues (2007) note that: “… for example, in terms of indices of scientific achievement, men were awarded 545 out of the 557 Nobel prizes awarded for science.” On the “idiot” end of the scale: there are a lot more men than women in prison, and one common denominator of prison inmates is that they tend to score very low on intelligence tests. (This is not to say that all criminals have low intelligence; perhaps mostly the ones that get caught do.)
Having said that, it is important to acknowledge that there are multiple types of intelligence, and even multi-indicator intelligence coefficients are usually poor approximations of an overall measure of intelligence (if there is one). This does not invalidate the main point of this post, which is related to score variability.
The table below (from: Deary and colleagues, 2007; click on it to enlarge; full reference at the end of this post) shows scores obtained by men and women (1,292 pairs of opposite-sex siblings) in various subtests of the Armed Services Vocational Aptitude Battery (ASVAB) test.
Note that nearly all of the differences between means (i.e., averages) are significant, but the direction of the differences (captured by the signs of the Cohen’s d coefficients, which are measures of effect size) varies a lot. That is, on several subtests (e.g., “Arithmetic”) men score higher, but in others (e.g., “Numerical operations”) women score higher. It all comes down to men and women scoring equally well overall.
Now look at the columns showing the standard deviations (“SD”) for men and women. In all subtests but two (“Coding speed” and “Numerical operations”) the standard deviation is higher for men; in many cases significantly higher (e.g., 44 percent higher for “Mechanical comprehension”). The standard deviations are about the same for “Coding speed” and “Numerical operations”. What this means is that variability in scores is nearly always higher, often significantly higher, among men than among women. I prepared the schematic figure below to illustrate the effect that this has on the numbers of individuals at the extremes.
The figure above shows two (badly drawn) quasi-normal distributions of scores. (This post shows a better illustration of a normal distribution.) The red curve refers to a distribution with a lower standard deviation than the blue curve; the latter is flatter. Each point on a curve reflects the number of individuals obtaining a particular score, which would be indicated on the horizontal axis. The number of individuals with that score is on the vertical axis. As you can see, the numbers of individuals scoring very high and low (geniuses and idiots, if the scores reflected intelligence) are greater for the blue curve, which is the curve with the higher standard deviation (higher dispersion of scores). The farther one goes to the left or right (the extremes), the bigger this difference becomes.
What does this have to do with evolution?
Well, there are a few possibilities, two of which appear to be particularly compelling. Maybe this effect is due to a combination of these two.
One is that ancestral women, like women today, selected mating partners based on a wide range of traits. Ancestral men on the other hand, like modern men, focused on a much smaller set of traits (Buss, 1995). The end result is more variation in traits, generally speaking, among men than among women. This refers to traits in general, not only intelligence. For example, there seems to be more variation in height among men than among women.
The other possible explanation is that, in our ancestral past, staying out of the extremes of intelligence was associated with higher survival success in both sexes. It seems that the incidence of certain types of mental disease (e.g., schizophrenia) is quite high among geniuses. This leads to more deaths due to related issues – suicide, depression leading to the metabolic syndrome, etc. And this is today, where geniuses can find many opportunities to “shine” in our complex urban societies. In our ancestral past the cognitive demands would have been much lower, and so would the practical value of being a genius.
If staying out of the extremes has indeed enhanced survival success in our evolutionary past, then it is reasonable to expect more women to fit that pattern than men. As with almost any “thing” that enhances survival success, women (especially pre-menopausal) naturally have more of that “thing” than men (e.g., HDL cholesterol).
The reason is that women are more important for the survival of any population than men; today and 1 million years ago. A population of 99 women and 1 man can potentially generate 99 children every few years. Here inbreeding in subsequent generations will be a problem, but that is better than extinction. A population with 99 women and 99 men (or even 1,000 men) will not generate significantly more children.
Reference:
Buss, D.M. (2003). The evolution of desire: Strategies of human mating. New York, NY: Basic Books.
Deary, I.J., Irwing, P., Der, G., & Bates, T.C. (2007). Brother–sister differences in the g factor in intelligence: Analysis of full, opposite-sex siblings from the NLSY1979. Intelligence, 35(5), 451-456.
What makes the study by Deary and colleagues (2007) particularly interesting is that its participants were opposite-sex siblings. This helped control for the influence of environmental factors. The downside is that the effect sizes might have been decreased, because of the high gene correlation among siblings, so we could expect larger differences between unrelated groups of men women. The differences, as you will see, are not in overall scores, but in score dispersion.
Let us get straight to the point made by the study. On average, men and women seem to score equally well on intelligence tests. The main difference is that there is more variation in the scores achieved by men than by women, which leads to an interesting effect: there are more geniuses and more idiots among men than among women.
This does NOT mean that a man’s genius is of a higher order; just that there is a tendency for more men to be geniuses (and idiots) than women in any random population sample. The women who are geniuses can be super geniuses, like two-time Nobel Prize winner Marie Curie, the first PERSON to receive such an honor. Albert Einstein is said that have greatly admired her intelligence.
As an illustration of this score dispersion effect, Deary and colleagues (2007) note that: “… for example, in terms of indices of scientific achievement, men were awarded 545 out of the 557 Nobel prizes awarded for science.” On the “idiot” end of the scale: there are a lot more men than women in prison, and one common denominator of prison inmates is that they tend to score very low on intelligence tests. (This is not to say that all criminals have low intelligence; perhaps mostly the ones that get caught do.)
Having said that, it is important to acknowledge that there are multiple types of intelligence, and even multi-indicator intelligence coefficients are usually poor approximations of an overall measure of intelligence (if there is one). This does not invalidate the main point of this post, which is related to score variability.
The table below (from: Deary and colleagues, 2007; click on it to enlarge; full reference at the end of this post) shows scores obtained by men and women (1,292 pairs of opposite-sex siblings) in various subtests of the Armed Services Vocational Aptitude Battery (ASVAB) test.
Note that nearly all of the differences between means (i.e., averages) are significant, but the direction of the differences (captured by the signs of the Cohen’s d coefficients, which are measures of effect size) varies a lot. That is, on several subtests (e.g., “Arithmetic”) men score higher, but in others (e.g., “Numerical operations”) women score higher. It all comes down to men and women scoring equally well overall.
Now look at the columns showing the standard deviations (“SD”) for men and women. In all subtests but two (“Coding speed” and “Numerical operations”) the standard deviation is higher for men; in many cases significantly higher (e.g., 44 percent higher for “Mechanical comprehension”). The standard deviations are about the same for “Coding speed” and “Numerical operations”. What this means is that variability in scores is nearly always higher, often significantly higher, among men than among women. I prepared the schematic figure below to illustrate the effect that this has on the numbers of individuals at the extremes.
The figure above shows two (badly drawn) quasi-normal distributions of scores. (This post shows a better illustration of a normal distribution.) The red curve refers to a distribution with a lower standard deviation than the blue curve; the latter is flatter. Each point on a curve reflects the number of individuals obtaining a particular score, which would be indicated on the horizontal axis. The number of individuals with that score is on the vertical axis. As you can see, the numbers of individuals scoring very high and low (geniuses and idiots, if the scores reflected intelligence) are greater for the blue curve, which is the curve with the higher standard deviation (higher dispersion of scores). The farther one goes to the left or right (the extremes), the bigger this difference becomes.
What does this have to do with evolution?
Well, there are a few possibilities, two of which appear to be particularly compelling. Maybe this effect is due to a combination of these two.
One is that ancestral women, like women today, selected mating partners based on a wide range of traits. Ancestral men on the other hand, like modern men, focused on a much smaller set of traits (Buss, 1995). The end result is more variation in traits, generally speaking, among men than among women. This refers to traits in general, not only intelligence. For example, there seems to be more variation in height among men than among women.
The other possible explanation is that, in our ancestral past, staying out of the extremes of intelligence was associated with higher survival success in both sexes. It seems that the incidence of certain types of mental disease (e.g., schizophrenia) is quite high among geniuses. This leads to more deaths due to related issues – suicide, depression leading to the metabolic syndrome, etc. And this is today, where geniuses can find many opportunities to “shine” in our complex urban societies. In our ancestral past the cognitive demands would have been much lower, and so would the practical value of being a genius.
If staying out of the extremes has indeed enhanced survival success in our evolutionary past, then it is reasonable to expect more women to fit that pattern than men. As with almost any “thing” that enhances survival success, women (especially pre-menopausal) naturally have more of that “thing” than men (e.g., HDL cholesterol).
The reason is that women are more important for the survival of any population than men; today and 1 million years ago. A population of 99 women and 1 man can potentially generate 99 children every few years. Here inbreeding in subsequent generations will be a problem, but that is better than extinction. A population with 99 women and 99 men (or even 1,000 men) will not generate significantly more children.
Reference:
Buss, D.M. (2003). The evolution of desire: Strategies of human mating. New York, NY: Basic Books.
Deary, I.J., Irwing, P., Der, G., & Bates, T.C. (2007). Brother–sister differences in the g factor in intelligence: Analysis of full, opposite-sex siblings from the NLSY1979. Intelligence, 35(5), 451-456.
Labels:
evolution,
intelligence,
mating,
research,
survival
Wednesday, April 21, 2010
Interesting links
Below is a list of links to web sites that deal with health issues in general. I have moved them from the previous “favorite links” area to this post so that I could save some space on the main page of the blog. Some of them are excellent sources of research-based and reliable information. Others are somewhat light in content, but still interesting. I certainly do not agree with the ideas espoused by all of them.
Alan Aragon
http://www.alanaragon.com/
Animal Pharm
http://drbganimalpharm.blogspot.com/
Ancestralize Me!
http://www.ancestralizeme.com/
Anthony Colpo
http://anthonycolpo.com/
Arthur De Vany
http://www.arthurdevany.com/
At Darwin's Table
http://darwinstable.wordpress.com/
Athletics by Nature
http://gregcarver.com/blog
Barefoot Ted's Adventures
http://barefootted.com/
Beef and Whiskey
http://beefandwhiskey.com/
Big Muscles Fast
http://www.bigmusclesfast.com/
Blaine's Low Carb Kitchen
http://fittv.discovery.com/fansites/blaine/recipes/recipes.html
Blood Sugar 101
http://www.phlaunt.com/diabetes
Brad Pilon's Blog
http://bradpilon.com/
Canibais e Reis
http://www.canibaisereis.com/
Cholesterol and Health
http://www.cholesterol-and-health.com/
Colorado State University's Physiologic Effects of Insulin
http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/pancreas/insulin_phys.html
Conditioning Research
http://conditioningresearch.blogspot.com/
Cooling Inflammation
http://coolinginflammation.blogspot.com/
Cut the Carb
http://www.cutthecarb.com/
David Mendosa
http://www.healthcentral.com/diabetes/c/17
Diabetes Update
http://diabetesupdate.blogspot.com/
Diet Doctor
http://www.dietdoctor.com
Discover Magazine Online
http://discovermagazine.com/
Dr. Bernstein's Diabetes Solution
http://diabetes-book.com/
Dr. Gabe Mirkin
http://www.drmirkin.com/
Dr. Michael R. Eades
http://www.proteinpower.com/drmike
Dr. Nemechek's Integrative Medicine
http://www.nemechekconsultativemedicine.com
Dr. Ron Rosedale
http://www.drrosedale.com/
Entropy Production
http://entropyproduction.blogspot.com/
Ernestine Shepherd
http://ernestineshepherd.net
Evolution for Everyone
http://scienceblogs.com/evolution/
Evolutionary Psychiatry
http://evolutionarypsychiatry.blogspot.com/
Evolving Thoughts by John Wilkins
http://evolvingthoughts.net
Exercise Prescription on the Net
http://www.exrx.net/
Experiments in Lifestyle Design by Tim Ferriss
http://www.fourhourworkweek.com/blog/
Fat Head
http://www.fathead-movie.com/
Fit 2 Fat 2 Fit
http://www.fit2fat2fit.com
Free the Animal
http://freetheanimal.com/
Grassroots Health
http://www.grassrootshealth.net/
Girl Gone Primal
http://girlgoneprimal.blogspot.com/
Gnolls by J. Stanton
http://www.gnolls.org
Health News Review
http://healthnewsreview.org/
Healthcare Epistemocrat
http://epistemocrat.blogspot.com/
Heretic
http://stan-heretic.blogspot.com/
Homo Consumericus
http://www.psychologytoday.com/blog/homo-consumericus
Hunt, Gather, Love
http://huntgatherlove.com/
Hunter Gatherer
http://hunter-gatherer.com/
Hyperlipid
http://high-fat-nutrition.blogspot.com/
ItsTheWooo's The Scribble Pad
http://itsthewooo.blogspot.com/
John Hawks Weblog
http://johnhawks.net/weblog
Julianne's Paleo & Zone Nutrition Blog
http://paleozonenutrition.wordpress.com/
Lean Gains
http://www.leangains.com/
Low-Carb for You
http://lowcarb4u.blogspot.com/
Lucas Tafur
http://www.lucastafur.com
Mark's Daily Apple
http://www.marksdailyapple.com/
Matt Metzgar's Blog
http://www.mattmetzgar.com/
Maxwell Murphy
http://maxwellmurphy.typepad.com/
Metabolism Society
http://nmsociety.org/
Michael Barker's Type 2 Ketosis Prone Diabetes
http://ketosisprone.blogspot.com/
Muscle and the City
http://www.muscleandthecity.com/
MuscleHack
http://www.musclehack.com/
My Carb Sane-Asylum
http://carbsanity.blogspot.com/
My Carb Sane Chronicles
http://carbsanitychronicles.blogspot.com/
Natural Messiah
http://naturalmessiah.blogspot.com/
Nephropal
http://nephropal.blogspot.com/
Nigee's Diet & Nutrition Blog
http://nigeepoo.blogspot.com/
Nourishing by Heart
http://lunchwithouted.wordpress.com/
Nutrition and Physical Regeneration
http://nutrition-and-physical-regeneration.com/blog
Nutrition, Health & Heart Disease
http://www.health-heart.org/
Omega-6 Fat News Commentary
http://omega-6-omega-3-balance.omegaoptimize.com/
Paleo Clinic
http://paleoclinic.blogspot.com/
Paleo Diet
http://paleodiet.com/
Paleo Hacks
http://paleohacks.com/
PaleoFitMD
http://paleofitmd.tumblr.com/
Patrick Ward's Optimum Sports Performance
http://optimumsportsperformance.com/blog/
Pay Now Live Later
http://paynowlivelater.blogspot.com/
Philosophy of Weight Management
http://philosophyofweightmanagement.blogspot.com
Prague Stepchild
http://praguestepchild.blogspot.com/
Primal Montain
http://www.primalmountain.com/c/blog/
Primal Wisdom
http://donmatesz.blogspot.com/
Principle Into Practice
http://principleintopractice.com
Protein Power
http://www.proteinpower.com/
PāNu
http://www.paleonu.com/
Rambling Outside the Box
http://ramblingoutsidethebox.blogspot.com/
Ramblings of a Carnivore
http://ramblingsofacarnivore.blogspot.com/
Raw Food SOS
http://rawfoodsos.com/
Ray Peat
http://raypeat.com/
Robb Wolf
http://robbwolf.com/
Ron Brown's The Myth of Loose Skin
http://www.bodyfatguide.com/LooseSkin.htm
Sandwalk by Laurence Moran
http://sandwalk.blogspot.com
Scooby's Home Bodybuilding Workouts
http://www.scoobysworkshop.com/
Seth Roberts's Blog
http://blog.sethroberts.net
Skyler Tanner
http://skylertanner.com
Sock Doc - Natural Injury Treatment & Prevention
http://sock-doc.com
Son of Grok
http://www.sonofgrok.com/
Spark of Reason
http://sparkofreason.blogspot.com/
Stella Style
http://stellastyle.com/
Survivorman - Discovery
http://dsc.discovery.com/fansites/survivorman/survivorman.html
That Paleo Guy
http://thatpaleoguy.com
The Carnivore Health Weblog
http://www.carnivorehealth.com
The Daily Lipid
http://www.cholesterol-and-health.com/cholesterol-blog.html
The Evolution & Medicine Review
http://evmedreview.com/
The Heart Scan
http://heartscanblog.blogspot.com/
The Healthy Skeptic
http://thehealthyskeptic.org/
The Livin' La Vida Low-Carb Show
http://www.thelivinlowcarbshow.com/shownotes
The Paleo Diet
http://www.thepaleodiet.com/
The Weston A. Price Foundation
http://www.westonaprice.org/
Theory to Practice
http://theorytopractice.wordpress.com/
Vitamin D Council
http://www.vitamindcouncil.org/
Vitamin D Wiki
http://www.vitamindwiki.com/
Weightology
http://weightology.net/
Whole Health Source
http://wholehealthsource.blogspot.com/
Wikipedia - Strength Training
http://en.wikipedia.org/wiki/Strength_training
Wildly Fluctuating
http://wildlyfluctuating.blogspot.com/
Zero Currency, Moneyless World - By Daniel Suelo
http://zerocurrency.blogspot.com/
Zeroing in on Recovery
http://malpaz.wordpress.com/
Zoe Harcombe
http://www.zoeharcombe.com/
180 Degree Health
http://180degreehealth.blogspot.com/
Alan Aragon
http://www.alanaragon.com/
Animal Pharm
http://drbganimalpharm.blogspot.com/
Ancestralize Me!
http://www.ancestralizeme.com/
Anthony Colpo
http://anthonycolpo.com/
Arthur De Vany
http://www.arthurdevany.com/
At Darwin's Table
http://darwinstable.wordpress.com/
Athletics by Nature
http://gregcarver.com/blog
Barefoot Ted's Adventures
http://barefootted.com/
Beef and Whiskey
http://beefandwhiskey.com/
Big Muscles Fast
http://www.bigmusclesfast.com/
Blaine's Low Carb Kitchen
http://fittv.discovery.com/fansites/blaine/recipes/recipes.html
Blood Sugar 101
http://www.phlaunt.com/diabetes
Bob Delmonteque
http://www.bodyrecomposition.com/Brad Pilon's Blog
http://bradpilon.com/
Canibais e Reis
http://www.canibaisereis.com/
Cholesterol and Health
http://www.cholesterol-and-health.com/
Colorado State University's Physiologic Effects of Insulin
http://www.vivo.colostate.edu/hbooks/pathphys/endocrine/pancreas/insulin_phys.html
Conditioning Research
http://conditioningresearch.blogspot.com/
Cooling Inflammation
http://coolinginflammation.blogspot.com/
Cut the Carb
http://www.cutthecarb.com/
David Mendosa
http://www.healthcentral.com/diabetes/c/17
Diabetes Update
http://diabetesupdate.blogspot.com/
Diet Doctor
http://www.dietdoctor.com
Discover Magazine Online
http://discovermagazine.com/
Dr. Bernstein's Diabetes Solution
http://diabetes-book.com/
Dr. Gabe Mirkin
http://www.drmirkin.com/
Dr. Michael R. Eades
http://www.proteinpower.com/drmike
Dr. Nemechek's Integrative Medicine
http://www.nemechekconsultativemedicine.com
Dr. Ron Rosedale
http://www.drrosedale.com/
Entropy Production
http://entropyproduction.blogspot.com/
Ernestine Shepherd
http://ernestineshepherd.net
Evolution for Everyone
http://scienceblogs.com/evolution/
Evolutionary Psychiatry
http://evolutionarypsychiatry.blogspot.com/
Evolving Thoughts by John Wilkins
http://evolvingthoughts.net
Exercise Prescription on the Net
http://www.exrx.net/
Experiments in Lifestyle Design by Tim Ferriss
http://www.fourhourworkweek.com/blog/
Fat Head
http://www.fathead-movie.com/
Fit 2 Fat 2 Fit
http://www.fit2fat2fit.com
Free the Animal
http://freetheanimal.com/
Grassroots Health
http://www.grassrootshealth.net/
Girl Gone Primal
http://girlgoneprimal.blogspot.com/
Gnolls by J. Stanton
http://www.gnolls.org
Health News Review
http://healthnewsreview.org/
Healthcare Epistemocrat
http://epistemocrat.blogspot.com/
Heretic
http://stan-heretic.blogspot.com/
Homo Consumericus
http://www.psychologytoday.com/blog/homo-consumericus
Hunt, Gather, Love
http://huntgatherlove.com/
Hunter Gatherer
http://hunter-gatherer.com/
Hyperlipid
http://high-fat-nutrition.blogspot.com/
ItsTheWooo's The Scribble Pad
http://itsthewooo.blogspot.com/
John Hawks Weblog
http://johnhawks.net/weblog
Julianne's Paleo & Zone Nutrition Blog
http://paleozonenutrition.wordpress.com/
Lean Gains
http://www.leangains.com/
Low-Carb for You
http://lowcarb4u.blogspot.com/
Lucas Tafur
http://www.lucastafur.com
Mark's Daily Apple
http://www.marksdailyapple.com/
Matt Metzgar's Blog
http://www.mattmetzgar.com/
Maxwell Murphy
http://maxwellmurphy.typepad.com/
Metabolism Society
http://nmsociety.org/
Michael Barker's Type 2 Ketosis Prone Diabetes
http://ketosisprone.blogspot.com/
Muscle and the City
http://www.muscleandthecity.com/
MuscleHack
http://www.musclehack.com/
My Carb Sane-Asylum
http://carbsanity.blogspot.com/
My Carb Sane Chronicles
http://carbsanitychronicles.blogspot.com/
Natural Messiah
http://naturalmessiah.blogspot.com/
Nephropal
http://nephropal.blogspot.com/
Nigee's Diet & Nutrition Blog
http://nigeepoo.blogspot.com/
Nourishing by Heart
http://lunchwithouted.wordpress.com/
Nutrition and Physical Regeneration
http://nutrition-and-physical-regeneration.com/blog
Nutrition, Health & Heart Disease
http://www.health-heart.org/
Omega-6 Fat News Commentary
http://omega-6-omega-3-balance.omegaoptimize.com/
Paleo Clinic
http://paleoclinic.blogspot.com/
Paleo Diet
http://paleodiet.com/
Paleo Hacks
http://paleohacks.com/
PaleoFitMD
http://paleofitmd.tumblr.com/
Patrick Ward's Optimum Sports Performance
http://optimumsportsperformance.com/blog/
Pay Now Live Later
http://paynowlivelater.blogspot.com/
Philosophy of Weight Management
http://philosophyofweightmanagement.blogspot.com
Prague Stepchild
http://praguestepchild.blogspot.com/
Primal Montain
http://www.primalmountain.com/c/blog/
Primal Wisdom
http://donmatesz.blogspot.com/
Principle Into Practice
http://principleintopractice.com
Protein Power
http://www.proteinpower.com/
PāNu
http://www.paleonu.com/
Rambling Outside the Box
http://ramblingoutsidethebox.blogspot.com/
Ramblings of a Carnivore
http://ramblingsofacarnivore.blogspot.com/
Raw Food SOS
http://rawfoodsos.com/
Ray Peat
http://raypeat.com/
Robb Wolf
http://robbwolf.com/
Ron Brown's The Myth of Loose Skin
http://www.bodyfatguide.com/LooseSkin.htm
Sandwalk by Laurence Moran
http://sandwalk.blogspot.com
Scooby's Home Bodybuilding Workouts
http://www.scoobysworkshop.com/
Seth Roberts's Blog
http://blog.sethroberts.net
Skyler Tanner
http://skylertanner.com
Sock Doc - Natural Injury Treatment & Prevention
http://sock-doc.com
Son of Grok
http://www.sonofgrok.com/
Spark of Reason
http://sparkofreason.blogspot.com/
Stella Style
http://stellastyle.com/
Survivorman - Discovery
http://dsc.discovery.com/fansites/survivorman/survivorman.html
That Paleo Guy
http://thatpaleoguy.com
The Carnivore Health Weblog
http://www.carnivorehealth.com
The Daily Lipid
http://www.cholesterol-and-health.com/cholesterol-blog.html
The Evolution & Medicine Review
http://evmedreview.com/
The Heart Scan
http://heartscanblog.blogspot.com/
The Healthy Skeptic
http://thehealthyskeptic.org/
The Livin' La Vida Low-Carb Show
http://www.thelivinlowcarbshow.com/shownotes
The Paleo Diet
http://www.thepaleodiet.com/
The Paleo Diet Blog
http://www.westonaprice.org/
Theory to Practice
http://theorytopractice.wordpress.com/
Vitamin D Council
http://www.vitamindcouncil.org/
Vitamin D Wiki
http://www.vitamindwiki.com/
Weightology
http://weightology.net/
Whole Health Source
http://wholehealthsource.blogspot.com/
Wikipedia - Strength Training
http://en.wikipedia.org/wiki/Strength_training
Wildly Fluctuating
http://wildlyfluctuating.blogspot.com/
Zero Currency, Moneyless World - By Daniel Suelo
http://zerocurrency.blogspot.com/
Zeroing in on Recovery
http://malpaz.wordpress.com/
Zoe Harcombe
http://www.zoeharcombe.com/
180 Degree Health
http://180degreehealth.blogspot.com/
Labels:
links
Sunday, April 18, 2010
Dinner with Taubes, Eades and Hujoel
Gary Taubes gave a lecture at UW last Thursday. Thanks to all the Whole Health Source readers who showed up. Gary's talk was titled "Why We Get Fat: Adiposity 101 and the Alternative Hypothesis of Obesity". He was hosted by Dr. Philippe Hujoel, the UW epidemiologist and dentist who authored the paper "Dietary Carbohydrates and Dental-Systemic Diseases" (1).
Gary's first target was the commonly held idea that obesity is simply caused by eating too much and exercising too little, and thus the cure is to eat less and exercise more. He used numerous examples from both humans and animals to show that fat mass is biologically regulated, rather than being the passive result of voluntary behaviors such as eating and exercise. He presented evidence of cultures remaining lean despite a huge and continuous surplus of food, as long as they stayed on their traditional diet. He also described how they subsequently became obese and diabetic on industrial foods (the Pima, for example).
He then moved into what he feels is the biological cause of obesity: excessive insulin keeping fat from exiting fat cells. It's true that insulin is a storage hormone, at the cellular level. However, fat mass regulation involves a dynamic interplay between many different interlacing systems that determine both overall energy intake and expenditure, as well as local availability of nutrients at the tissue level (i.e., how much fat gets into your fat tissue vs. your muscle tissue). I think the cause of obesity is likely to be more complex than insulin signaling.
He also offered the "carbohydrate hypothesis", which is the idea that carbohydrate, or at least refined carbohydrate, is behind the obesity epidemic and perhaps other metabolic problems. This is due to its ability to elevate insulin. I agree that refined carbohydrate, particularly white flour and sugar, is probably a central part of the problem. I'm also open to the possibility that some people in industrial nations are genuinely sensitive to carbohydrate regardless of what form it's in, although that remains to be rigorously tested. I don't think carbohydrate is sufficient to cause obesity per se, due to the many lean and healthy cultures that eat high carbohydrate diets*. Gary acknowledges this, and thinks there's probably another factor that's involved in allowing carbohydrate sensitivity to develop, for example excessive sugar.
I had the opportunity to speak with Gary at length on Thursday, as well as on Friday at dinner. Gary is a very nice guy-- a straightforward New York personality who's not averse to a friendly disagreement. In case any of you are wondering, he looks good. Good body composition, nice skin, hair and teeth (apologies to Gary for the analysis). Philippe and his wife took us out to a very nice restaurant, where we had a leisurely four-hour meal, and Dr. Mike Eades was in town so he joined us as well. Mike has a strong Southern accent and is also a pleasant guy. Philippe and his wife are generous and engaging people. It was a great evening. The restaurant was nice enough that I wasn't going to be picky about the food-- I ate everything that was put in front of me and enjoyed it.
* I'm talking about prevention rather than cure here. I acknowledge that many people have had some success losing fat using low-carbohydrate diets, including two gentlemen I met on Thursday.
Gary's first target was the commonly held idea that obesity is simply caused by eating too much and exercising too little, and thus the cure is to eat less and exercise more. He used numerous examples from both humans and animals to show that fat mass is biologically regulated, rather than being the passive result of voluntary behaviors such as eating and exercise. He presented evidence of cultures remaining lean despite a huge and continuous surplus of food, as long as they stayed on their traditional diet. He also described how they subsequently became obese and diabetic on industrial foods (the Pima, for example).
He then moved into what he feels is the biological cause of obesity: excessive insulin keeping fat from exiting fat cells. It's true that insulin is a storage hormone, at the cellular level. However, fat mass regulation involves a dynamic interplay between many different interlacing systems that determine both overall energy intake and expenditure, as well as local availability of nutrients at the tissue level (i.e., how much fat gets into your fat tissue vs. your muscle tissue). I think the cause of obesity is likely to be more complex than insulin signaling.
He also offered the "carbohydrate hypothesis", which is the idea that carbohydrate, or at least refined carbohydrate, is behind the obesity epidemic and perhaps other metabolic problems. This is due to its ability to elevate insulin. I agree that refined carbohydrate, particularly white flour and sugar, is probably a central part of the problem. I'm also open to the possibility that some people in industrial nations are genuinely sensitive to carbohydrate regardless of what form it's in, although that remains to be rigorously tested. I don't think carbohydrate is sufficient to cause obesity per se, due to the many lean and healthy cultures that eat high carbohydrate diets*. Gary acknowledges this, and thinks there's probably another factor that's involved in allowing carbohydrate sensitivity to develop, for example excessive sugar.
I had the opportunity to speak with Gary at length on Thursday, as well as on Friday at dinner. Gary is a very nice guy-- a straightforward New York personality who's not averse to a friendly disagreement. In case any of you are wondering, he looks good. Good body composition, nice skin, hair and teeth (apologies to Gary for the analysis). Philippe and his wife took us out to a very nice restaurant, where we had a leisurely four-hour meal, and Dr. Mike Eades was in town so he joined us as well. Mike has a strong Southern accent and is also a pleasant guy. Philippe and his wife are generous and engaging people. It was a great evening. The restaurant was nice enough that I wasn't going to be picky about the food-- I ate everything that was put in front of me and enjoyed it.
* I'm talking about prevention rather than cure here. I acknowledge that many people have had some success losing fat using low-carbohydrate diets, including two gentlemen I met on Thursday.
Labels:
overweight
Ketones and Ketosis: Physiological and pathological forms
Ketones are compounds that have a specific chemical structure. The figure below (from: Wikipedia) shows the chemical structure of various types of ketones. As you can see, all ketones share a carbonyl group; that is the “O=” part of their chemical structure. A carbonyl group is an oxygen atom double-bonded to a carbon atom.
Technically speaking, many substances can be classified as ketones. Not all of these are involved in the same metabolic processes in humans. For example, fructose is technically a ketone, but it is not one of the three main ketones produced by humans from dietary macronutrients (discussed below), and is not metabolized in the same way as are those three main ketones.
Humans, as well as most other vertebrates, produce three main ketones (also known as ketone bodies) from dietary macronutrients. These are acetone, acetoacetate and beta-hydroxybutyrate. Low carbohydrate diets tend to promote glycogen depletion, which in turn leads to increased production of these ketones. Glycogen is stored in the liver and muscles. Liver glycogen is used by the body to maintain blood glucose levels within a narrow range in the fasted state. Examples of diets that tend to promote glycogen depletion are the Atkins Diet and Kwaśniewski’s Optimal Diet.
A search for articles on ketosis in scientific databases usually returns a large number of articles dealing with ketosis in cows. Why? The reason is that ketosis reduces milk production, by both reducing the amount of fat and glucose available for milk synthesis. In fact, ketosis is referred to as a “disease” in cows.
In humans, most articles on ketosis refer to pathological ketosis (a.k.a. ketoacidosis), especially in the context of uncontrolled diabetes. One notable exception is an article by Williamson (2005), from which the table below was taken. The table shows ketone concentrations in the blood under various circumstances, in mmol/l.
As you can see, relatively high concentrations of ketones occur in newborn babies (neonate), in adults post-exercise, and in adults fed a high fat diet. Generally speaking, a high fat diet is a low carbohydrate diet, and a high carbohydrate diet is a low fat diet. (One occasionally sees diets that are high in both carbohydrates and fat; which seem excellent at increasing body fat and thus reducing life span. This diet is apparently popular among sumo wrestlers, where genetics and vigorous exercise usually counter the negative diet effects.)
Situations in which ketosis occurs in newborn babies (neonate), in adults post-exercise, and in adults fed a high fat diet are all examples of physiological, or benign, ketosis. Ketones are also found in low concentrations in adults fed a standard American diet.
Ketones are found in very high concentrations in adults with untreated diabetes. This is an example of pathological ketosis, even though ketones are produced as part of a protective compensatory mechanism to spare glucose for the brain and red blood cells (which need glucose to function properly). Pathological ketosis leads to serum ketone levels that can be as much as 80 times (or more) those found in physiological ketosis.
Serum ketone concentrations increase proportionally to decreases in stored glycogen and, when glycogen is low or absent, correlate strongly (and inversely) with blood glucose levels. In some individuals glycogen is practically absent due to a genetic condition that leads to hepatic glycogen synthase deficiency. This is a deficiency of the enzyme that promotes glycogen synthesis by the liver. The figure below (also from Williamson, 2005) shows the variations in glucose and ketone levels in a child with glycogen synthase deficiency.
What happened with this child? Williamson answers this question: “It is of interest that this particular child suffered no ill effects from the daily exposure to high concentrations of ketone bodies, underlining their role as normal substrates for the brain when available.”
Unlike glucose and lipoprotein-bound fats (in VLDL, for example), unused ketones cannot be converted back to substances that can be stored by the body. Thus excess ketones are eliminated in the urine; leading to their detection by various tests, e.g., Ketostix tests. This elimination of unused ketones in the urine is one of the reasons why low carbohydrate diets are believed to lead to enhanced body fat loss.
In summary, ketones are present in the blood most of the time, in most people, whether they are on a ketogenic diet or not. If they do not show up in the urine, it does not mean that they are not present in the blood; although it usually means that their concentration in the blood is not that high. Like glucose, ketones are soluble in water, and thus circulate in the blood without the need for carriers (e.g., albumin, which is needed for the transport of free fatty acids; and VLDL, needed for the transport of triglycerides). Like glucose, they are used as sources of energy by the brain and by muscle tissues.
It has been speculated that ketosis leads to accelerated aging, through the formation of advanced glycation endproducts (AGEs), a speculation that seems to be largely unfounded (see this post). It is difficult to believe that a metabolic process that is universally found in babies and adults post-exercise would have been favored by evolution if it led to accelerated aging.
References:
Williamson, D.H. (2005). Ketosis. Encyclopedia of Human Nutrition, 91-98.
Technically speaking, many substances can be classified as ketones. Not all of these are involved in the same metabolic processes in humans. For example, fructose is technically a ketone, but it is not one of the three main ketones produced by humans from dietary macronutrients (discussed below), and is not metabolized in the same way as are those three main ketones.
Humans, as well as most other vertebrates, produce three main ketones (also known as ketone bodies) from dietary macronutrients. These are acetone, acetoacetate and beta-hydroxybutyrate. Low carbohydrate diets tend to promote glycogen depletion, which in turn leads to increased production of these ketones. Glycogen is stored in the liver and muscles. Liver glycogen is used by the body to maintain blood glucose levels within a narrow range in the fasted state. Examples of diets that tend to promote glycogen depletion are the Atkins Diet and Kwaśniewski’s Optimal Diet.
A search for articles on ketosis in scientific databases usually returns a large number of articles dealing with ketosis in cows. Why? The reason is that ketosis reduces milk production, by both reducing the amount of fat and glucose available for milk synthesis. In fact, ketosis is referred to as a “disease” in cows.
In humans, most articles on ketosis refer to pathological ketosis (a.k.a. ketoacidosis), especially in the context of uncontrolled diabetes. One notable exception is an article by Williamson (2005), from which the table below was taken. The table shows ketone concentrations in the blood under various circumstances, in mmol/l.
As you can see, relatively high concentrations of ketones occur in newborn babies (neonate), in adults post-exercise, and in adults fed a high fat diet. Generally speaking, a high fat diet is a low carbohydrate diet, and a high carbohydrate diet is a low fat diet. (One occasionally sees diets that are high in both carbohydrates and fat; which seem excellent at increasing body fat and thus reducing life span. This diet is apparently popular among sumo wrestlers, where genetics and vigorous exercise usually counter the negative diet effects.)
Situations in which ketosis occurs in newborn babies (neonate), in adults post-exercise, and in adults fed a high fat diet are all examples of physiological, or benign, ketosis. Ketones are also found in low concentrations in adults fed a standard American diet.
Ketones are found in very high concentrations in adults with untreated diabetes. This is an example of pathological ketosis, even though ketones are produced as part of a protective compensatory mechanism to spare glucose for the brain and red blood cells (which need glucose to function properly). Pathological ketosis leads to serum ketone levels that can be as much as 80 times (or more) those found in physiological ketosis.
Serum ketone concentrations increase proportionally to decreases in stored glycogen and, when glycogen is low or absent, correlate strongly (and inversely) with blood glucose levels. In some individuals glycogen is practically absent due to a genetic condition that leads to hepatic glycogen synthase deficiency. This is a deficiency of the enzyme that promotes glycogen synthesis by the liver. The figure below (also from Williamson, 2005) shows the variations in glucose and ketone levels in a child with glycogen synthase deficiency.
What happened with this child? Williamson answers this question: “It is of interest that this particular child suffered no ill effects from the daily exposure to high concentrations of ketone bodies, underlining their role as normal substrates for the brain when available.”
Unlike glucose and lipoprotein-bound fats (in VLDL, for example), unused ketones cannot be converted back to substances that can be stored by the body. Thus excess ketones are eliminated in the urine; leading to their detection by various tests, e.g., Ketostix tests. This elimination of unused ketones in the urine is one of the reasons why low carbohydrate diets are believed to lead to enhanced body fat loss.
In summary, ketones are present in the blood most of the time, in most people, whether they are on a ketogenic diet or not. If they do not show up in the urine, it does not mean that they are not present in the blood; although it usually means that their concentration in the blood is not that high. Like glucose, ketones are soluble in water, and thus circulate in the blood without the need for carriers (e.g., albumin, which is needed for the transport of free fatty acids; and VLDL, needed for the transport of triglycerides). Like glucose, they are used as sources of energy by the brain and by muscle tissues.
It has been speculated that ketosis leads to accelerated aging, through the formation of advanced glycation endproducts (AGEs), a speculation that seems to be largely unfounded (see this post). It is difficult to believe that a metabolic process that is universally found in babies and adults post-exercise would have been favored by evolution if it led to accelerated aging.
References:
Williamson, D.H. (2005). Ketosis. Encyclopedia of Human Nutrition, 91-98.
Thursday, April 15, 2010
Copper in Food
Sources of Copper
It isn't hard to get enough copper-- unless you eat an industrial diet. I've compiled a chart showing the copper content of various refined and unrefined foods to illustrate the point. The left side shows industrial staple foods, while the right side shows whole foods. I've incorporated a few that would have been typical of Polynesian and Melanesian cultures apparently free of cardiovascular disease. The serving sizes are what one might reasonably eat at a meal: roughly 200 calories for grains, tubers and whole coconut; 1/4 pound for animal products; 1/2 teaspoon for salt; 1 cup for raw kale; 1 oz for sugar.
 Note that beef liver is off the chart at 488 percent of the USDA recommended daily allowance. I don't know if you'd want to sit down and eat a quarter pound of beef liver, but you get the picture. Beef liver is nature's multivitamin: hands down the Most Nutritious Food in the World. That's because it acts as a storage depot for a number of important micronutrients, as well as being a biochemical factory that requires a large amount of B vitamins to function. You can see that muscle tissue isn't a great source of copper compared to other organs.
Note that beef liver is off the chart at 488 percent of the USDA recommended daily allowance. I don't know if you'd want to sit down and eat a quarter pound of beef liver, but you get the picture. Beef liver is nature's multivitamin: hands down the Most Nutritious Food in the World. That's because it acts as a storage depot for a number of important micronutrients, as well as being a biochemical factory that requires a large amount of B vitamins to function. You can see that muscle tissue isn't a great source of copper compared to other organs.
Beef liver is so full of micronutrients, it shouldn't be eaten every day. Think of it in terms of the composition of a cow's body. The edible carcass is mostly muscle, but a significant portion is liver. I think it makes sense to eat some form of liver about once per week.
Modern Agriculture Produces Micronutrient-poor Foods
The numbers in the graph above come from NutritionData, my main source of food nutrient composition. The problem with relying on this kind of information is it ignores the variability in micronutrient content due to plant strain, soil quality, et cetera.
The unfortunate fact is that micronutrient levels have declined substantially over the course of the 20th century, even in whole foods. Dr. Donald R. Davis has documented the substantial decline in copper and other micronutrients in American foods over the second half of the last century (1). An even more marked decrease has occurred in the UK (2), with similar trends worldwide. On average, the copper content of vegetables in the UK has declined 76 percent since 1940. Most of the decrease has taken place since 1978. Fruits are down 20 percent and meats are down 24 percent.
I find this extremely disturbing, as it will affect even people eating whole food diets. This is yet another reason to buy from artisanal producers, who are likely to use more traditional plant varieties and grow in richer soil. Grass-fed beef should be just as nutritious as it has always been. Some people may also wish to grow, hunt or fish their own food.
It isn't hard to get enough copper-- unless you eat an industrial diet. I've compiled a chart showing the copper content of various refined and unrefined foods to illustrate the point. The left side shows industrial staple foods, while the right side shows whole foods. I've incorporated a few that would have been typical of Polynesian and Melanesian cultures apparently free of cardiovascular disease. The serving sizes are what one might reasonably eat at a meal: roughly 200 calories for grains, tubers and whole coconut; 1/4 pound for animal products; 1/2 teaspoon for salt; 1 cup for raw kale; 1 oz for sugar.
 Note that beef liver is off the chart at 488 percent of the USDA recommended daily allowance. I don't know if you'd want to sit down and eat a quarter pound of beef liver, but you get the picture. Beef liver is nature's multivitamin: hands down the Most Nutritious Food in the World. That's because it acts as a storage depot for a number of important micronutrients, as well as being a biochemical factory that requires a large amount of B vitamins to function. You can see that muscle tissue isn't a great source of copper compared to other organs.
Note that beef liver is off the chart at 488 percent of the USDA recommended daily allowance. I don't know if you'd want to sit down and eat a quarter pound of beef liver, but you get the picture. Beef liver is nature's multivitamin: hands down the Most Nutritious Food in the World. That's because it acts as a storage depot for a number of important micronutrients, as well as being a biochemical factory that requires a large amount of B vitamins to function. You can see that muscle tissue isn't a great source of copper compared to other organs.Beef liver is so full of micronutrients, it shouldn't be eaten every day. Think of it in terms of the composition of a cow's body. The edible carcass is mostly muscle, but a significant portion is liver. I think it makes sense to eat some form of liver about once per week.
Modern Agriculture Produces Micronutrient-poor Foods
The numbers in the graph above come from NutritionData, my main source of food nutrient composition. The problem with relying on this kind of information is it ignores the variability in micronutrient content due to plant strain, soil quality, et cetera.
The unfortunate fact is that micronutrient levels have declined substantially over the course of the 20th century, even in whole foods. Dr. Donald R. Davis has documented the substantial decline in copper and other micronutrients in American foods over the second half of the last century (1). An even more marked decrease has occurred in the UK (2), with similar trends worldwide. On average, the copper content of vegetables in the UK has declined 76 percent since 1940. Most of the decrease has taken place since 1978. Fruits are down 20 percent and meats are down 24 percent.
I find this extremely disturbing, as it will affect even people eating whole food diets. This is yet another reason to buy from artisanal producers, who are likely to use more traditional plant varieties and grow in richer soil. Grass-fed beef should be just as nutritious as it has always been. Some people may also wish to grow, hunt or fish their own food.
Labels:
Cardiovascular disease,
diet,
liver,
minerals
Insulin responses to foods rich in carbohydrates and protein
Insulin is often presented as a hormone that is at the core of the diseases of civilization, particularly because of the insulin response elicited by foods rich in refined carbohydrates and sugars. What is often not mentioned is that protein also elicits an insulin response and so do foods where carbohydrates are mixed with fat. Sometimes the insulin responses are way more than one would expect based on the macronutrient compositions of the foods.
Holt et al. (1997; full reference at the end of this post) conducted a classic study of insulin responses. This study has been widely cited, and paints an interesting picture of differences in insulin responses to various foods. But you have to be careful where you look. There has been some confusion about the results because of the way they are often reported in places like Wikipedia and on various Internet sites that refer to the study.
The key thing to bear in mind when reviewing this study is that the amounts of food used were designed to have the same calorie content: 1000 kJ or 240 kcal (i.e., 240 calories). This led to wild variations in the size of the portions that are compared and their weight in grams. Also, some of the food portions are probably not what people usually eat in one sitting.
In Holt et al.’s (1997) study the participants were 41 lean and healthy university students. They were fed 1000 kJ (240 kcal) portions of the test foods on separate mornings after a 10-hour fast overnight. Blood insulin levels were measured at different times within a 120-minute period after each meal. An insulin score was then calculated from the area under the insulin response curve for each food; white bread was used as the reference food.
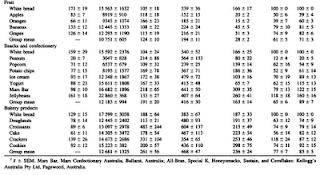
Part of Table 2 on page 1267 is shown below (the full text version of the paper is linked at the end of this post), just to illustrate the types and amounts of food served, and the macronutrient breakdown for each food. I hope you can see what I meant when I said that some of the food portions are probably not what people usually eat in one sitting. I don’t think it would be hard to find someone who would eat 158 g of beef steak in one sitting, but 333 g of fish is a little more difficult. Fish has a higher proportion of protein than beef steak, and thus is more satiating. The same goes for 625 g of orange, about 6 oranges. Foods that have more fat have more calories per gram; hence the smaller portions served for high-fat foods.
Table 4 of the article is a bit long, so I am providing it in two parts below. AUC stands for “area under the curve”. As you can see, for isocaloric portions of different foods (i.e., with the same amount of calories), there is a huge variation in insulin response. The insulin AUCs are shown on the second numeric column from the left. Also note that the insulin responses (AUC) for white bread varied in different meals. This complicates things a bit, but at least provides a more realistic view of the responses since each participant served as his or her own control.
Look at the third column from the right, which shows the insulin responses per gram of each food, compared with the response to white bread, always shown at the top for each group of related foods (e.g., protein-rich foods). The gram-adjusted response for whole-meal bread is rather high, and so is the glucose response. The gram-adjusted insulin response to potatoes is less than one-third of the response to white bread, even though the non-gram-adjusted glucose response is higher. The insulin response to beef is also less than one-third of the response to white bread, gram-for-gram. Even cheese leads to a gram-adjusted response that is about half the one for white bread, and I don’t think many people will eat the same amount of cheese in one sitting as they would do with white bread.
In summary, insulin responses to protein-rich foods are often 50 to 70 percent lower than responses to equivalent amounts of refined carbohydrate-rich foods. Also, insulin responses to unrefined carbohydrate-rich foods (e.g., potato, fruits) are often 70 to 90 percent lower than responses to equivalent amounts of refined carbohydrate-rich foods.
Why do insulin levels go up in response to dietary protein?
One of the reasons is that insulin is needed for tissue protein synthesis. That is, increased circulating protein (as amino acids) and insulin have a net anabolic effect, promoting muscle growth and inhibiting muscle breakdown. (Muscle protein synthesis and breakdown happen all the time; the net effect defines whether muscle grows or shrinks.) In this respect, insulin acts in conjunction with other hormones, such as growth hormone and insulin-like growth factor 1.
Reference:
Holt, S.H., Miller, J.C., & Petocz, P. (1997). An insulin index of foods: The insulin demand generated by 1000-kJ portions of common foods. American Journal of Clinical Nutrition, 66, 1264-1276.
Holt et al. (1997; full reference at the end of this post) conducted a classic study of insulin responses. This study has been widely cited, and paints an interesting picture of differences in insulin responses to various foods. But you have to be careful where you look. There has been some confusion about the results because of the way they are often reported in places like Wikipedia and on various Internet sites that refer to the study.
The key thing to bear in mind when reviewing this study is that the amounts of food used were designed to have the same calorie content: 1000 kJ or 240 kcal (i.e., 240 calories). This led to wild variations in the size of the portions that are compared and their weight in grams. Also, some of the food portions are probably not what people usually eat in one sitting.
In Holt et al.’s (1997) study the participants were 41 lean and healthy university students. They were fed 1000 kJ (240 kcal) portions of the test foods on separate mornings after a 10-hour fast overnight. Blood insulin levels were measured at different times within a 120-minute period after each meal. An insulin score was then calculated from the area under the insulin response curve for each food; white bread was used as the reference food.
Part of Table 2 on page 1267 is shown below (the full text version of the paper is linked at the end of this post), just to illustrate the types and amounts of food served, and the macronutrient breakdown for each food. I hope you can see what I meant when I said that some of the food portions are probably not what people usually eat in one sitting. I don’t think it would be hard to find someone who would eat 158 g of beef steak in one sitting, but 333 g of fish is a little more difficult. Fish has a higher proportion of protein than beef steak, and thus is more satiating. The same goes for 625 g of orange, about 6 oranges. Foods that have more fat have more calories per gram; hence the smaller portions served for high-fat foods.
Table 4 of the article is a bit long, so I am providing it in two parts below. AUC stands for “area under the curve”. As you can see, for isocaloric portions of different foods (i.e., with the same amount of calories), there is a huge variation in insulin response. The insulin AUCs are shown on the second numeric column from the left. Also note that the insulin responses (AUC) for white bread varied in different meals. This complicates things a bit, but at least provides a more realistic view of the responses since each participant served as his or her own control.
Look at the third column from the right, which shows the insulin responses per gram of each food, compared with the response to white bread, always shown at the top for each group of related foods (e.g., protein-rich foods). The gram-adjusted response for whole-meal bread is rather high, and so is the glucose response. The gram-adjusted insulin response to potatoes is less than one-third of the response to white bread, even though the non-gram-adjusted glucose response is higher. The insulin response to beef is also less than one-third of the response to white bread, gram-for-gram. Even cheese leads to a gram-adjusted response that is about half the one for white bread, and I don’t think many people will eat the same amount of cheese in one sitting as they would do with white bread.
In summary, insulin responses to protein-rich foods are often 50 to 70 percent lower than responses to equivalent amounts of refined carbohydrate-rich foods. Also, insulin responses to unrefined carbohydrate-rich foods (e.g., potato, fruits) are often 70 to 90 percent lower than responses to equivalent amounts of refined carbohydrate-rich foods.
Why do insulin levels go up in response to dietary protein?
One of the reasons is that insulin is needed for tissue protein synthesis. That is, increased circulating protein (as amino acids) and insulin have a net anabolic effect, promoting muscle growth and inhibiting muscle breakdown. (Muscle protein synthesis and breakdown happen all the time; the net effect defines whether muscle grows or shrinks.) In this respect, insulin acts in conjunction with other hormones, such as growth hormone and insulin-like growth factor 1.
Reference:
Holt, S.H., Miller, J.C., & Petocz, P. (1997). An insulin index of foods: The insulin demand generated by 1000-kJ portions of common foods. American Journal of Clinical Nutrition, 66, 1264-1276.
Tuesday, April 13, 2010
Long-term adherence to Dr. Kwaśniewski’s Optimal Diet: Healthy with high LDL cholesterol
This is a study (Grieb, P. et al., 2008; full reference at the end of this post) that I read a few years ago, right after it came out, and at the time I recall thinking about the apparent contradiction between the positive effects of the Optimal Diet and the very elevated LDL cholesterol levels among the participants. I say “contradiction” because of the established and misguided dogma among medical doctors, particularly general practitioners, that decreasing LDL cholesterol levels is the best strategy to avoid cardiovascular disease.
The Optimal Diet is one of the best examples of a healthy diet where LDL cholesterol levels are generally high, in fact much higher than most people are willing to accept as healthy today. (In this study, LDL cholesterol levels were calculated based on the Friedewald equation.)
It is not uncommon to see people concerned about their high LDL cholesterol levels after adopting a low carbohydrate diet. (A low carbohydrate diet is, generally speaking, a high fat diet.) This study shows that this is a rather common thing, and also that it is not something that those who experience it should be too concerned about. To be convinced of this, one can always do a VAP test (see this post for a link to a sample VAP test report) and check his or her LDL particle pattern.
The study presents the Optimal Diet as the Polish equivalent to the Atkins diet. It states that the Diet’s main characteristic is maintaining the proportion of proteins:fat:carbs. in the range of 1:2.5-3.5:0.5, with no restriction on the amount of food consumed. In fact, as you will see in this post, more than 70 percent of the calories consumed by the study participants came from fat.
Easily digestible carbohydrate-rich foods are not part of the Optimal Diet. More specifically, the following foods were listed as not being allowed in the Optimal Diet: sucrose, sweets, honey, jam, white rice, bread, starches in general, beans, potatoes (only in small amounts), and sweetened drinks. Also, the Optimal Diet is definitely a low carbohydrate diet, but not what is often referred to as a "very low carbohydrate diet". In this study, the typical carbohydrate intake per day was around 60 g.
Thirty-one healthy people participated in the study, 17 women and 14 men. The average age was 51.7 (standard deviation: 16.6). They had self-reportedly adhered to the Optimal Diet for at least 1 year prior to the study; the average period of adherence was 4.1 years (standard deviation: 1.9). So, the vast majority had been on the diet for more than 2.2 years, about half for 4.1 years or more, and about one-sixth for more than 6 years. (Check this post if you want to know how these figures can be calculated based on the average period of adherence and the standard deviation.)
The table below (click on it to enlarge) shows anthropometric and physiologic characteristics of the participants. Note that longer adherence to the Optimal Diet (right end of the table) was associated with lower systolic and diastolic blood pressure, as well as lower body mass index (BMI). (It was also associated with lower height and BMR, so I am guessing that more women tended to be long-term adherers than men.) Most of the participants had BMIs in the normal range, with only one in the obese category. That was a 43-year-old man who followed the diet for 1.5 years; he had a BMI of 34.1.
The macronutrient distribution of the Optimal Diet is shown on the table below (click on it to enlarge), as followed by the participants. As you can see, protein intake was not that high; about 53.9 g per day on average for men, a bit less for women. Note the percentage of calories from fat: more than 77 percent for men and 72 percent for women. Given the BMIs just discussed, one can safely say based on this that eating a lot of fat did not make the participants fat.
The table below (click on it to enlarge) has some interesting health markers. Note that free fatty acids (FFAs) were elevated. This is to be expected, as these folks were burning fat for energy most of the time, and not as much glucose. The FFAs are not really “free”, but bound to a protein called albumin, which is abundant in human blood. FFAs yield large quantities of adenosine triphosphate (ATP), the main energy “currency” used by the body.
These levels of FFAs are also usually associated with mild ketosis, where ketones are produced by the body and used for energy. Unlike albumin-bound FFAs, ketones are soluble in water, and thus circulate freely through the blood. The mild ketosis experienced by the participants was possibly to the point where ketones showed in the urine. The article mentions this, and provides a measure of beta-HB (beta-hydroxybutyrate, a ketone body), which is elevated as expected, but does not provide urine or other blood ketone measures (e.g., blood acetone levels). Also note the fairly healthy fasting glucose levels, slightly higher in men than in women, but fairly low overall. Fairly healthy insulin levels as well; at the high end of what Stephan at Whole Health Source would recommend, but still significantly lower than the average insulin level in the U.S. at the time of the article's publication.
Finally, the table below (click on it to enlarge) shows lipids and a few other measures. Total cholesterol was on average a bit more than 278 mg/dL. LDL cholesterol was a bit higher than 188 mg/dL on average; high enough to make most doctors cringe today. Based on the means and standard deviations provided, we can estimate that about 16 percent of the participants had LDL cholesterol levels higher than 228.1 mg/dL. About 2.5 percent of the participants had LDL cholesterol levels higher than 268 mg/dL. And this is all after adhering to the diet for a relatively long period of time; even higher LDL cholesterol levels might have occurred right after adoption.
Yet average HDL cholesterol was a very high and protective 71.6 mg/dL. This high HDL and the relatively low triglycerides suggest a large-buoyant non-atherogenic LDL particle pattern.
Average HOMA(IR), a measure of insulin resistance, was a low 1.35 mU/mmol; strongly indicating, together with the relatively low fasting glucose levels, that the participants were far from being pre-diabetic, let alone diabetic.
Diabetes is a strong risk factor for cardiovascular disease, and many other health complications; much more so than elevated LDL cholesterol.
The Optimal Diet does not seem to be a diet for bodybuilders, but I would say that, overall, Peter at Hyperlipid has chosen a diet that makes some sense.
Reference:
Grieb, P. et al. (2008). Long-term consumption of a carbohydrate-restricted diet does not induce deleterious metabolic effects. Nutrition Research, 28(12), 825-833.
The Optimal Diet is one of the best examples of a healthy diet where LDL cholesterol levels are generally high, in fact much higher than most people are willing to accept as healthy today. (In this study, LDL cholesterol levels were calculated based on the Friedewald equation.)
It is not uncommon to see people concerned about their high LDL cholesterol levels after adopting a low carbohydrate diet. (A low carbohydrate diet is, generally speaking, a high fat diet.) This study shows that this is a rather common thing, and also that it is not something that those who experience it should be too concerned about. To be convinced of this, one can always do a VAP test (see this post for a link to a sample VAP test report) and check his or her LDL particle pattern.
The study presents the Optimal Diet as the Polish equivalent to the Atkins diet. It states that the Diet’s main characteristic is maintaining the proportion of proteins:fat:carbs. in the range of 1:2.5-3.5:0.5, with no restriction on the amount of food consumed. In fact, as you will see in this post, more than 70 percent of the calories consumed by the study participants came from fat.
Easily digestible carbohydrate-rich foods are not part of the Optimal Diet. More specifically, the following foods were listed as not being allowed in the Optimal Diet: sucrose, sweets, honey, jam, white rice, bread, starches in general, beans, potatoes (only in small amounts), and sweetened drinks. Also, the Optimal Diet is definitely a low carbohydrate diet, but not what is often referred to as a "very low carbohydrate diet". In this study, the typical carbohydrate intake per day was around 60 g.
Thirty-one healthy people participated in the study, 17 women and 14 men. The average age was 51.7 (standard deviation: 16.6). They had self-reportedly adhered to the Optimal Diet for at least 1 year prior to the study; the average period of adherence was 4.1 years (standard deviation: 1.9). So, the vast majority had been on the diet for more than 2.2 years, about half for 4.1 years or more, and about one-sixth for more than 6 years. (Check this post if you want to know how these figures can be calculated based on the average period of adherence and the standard deviation.)
The table below (click on it to enlarge) shows anthropometric and physiologic characteristics of the participants. Note that longer adherence to the Optimal Diet (right end of the table) was associated with lower systolic and diastolic blood pressure, as well as lower body mass index (BMI). (It was also associated with lower height and BMR, so I am guessing that more women tended to be long-term adherers than men.) Most of the participants had BMIs in the normal range, with only one in the obese category. That was a 43-year-old man who followed the diet for 1.5 years; he had a BMI of 34.1.
The macronutrient distribution of the Optimal Diet is shown on the table below (click on it to enlarge), as followed by the participants. As you can see, protein intake was not that high; about 53.9 g per day on average for men, a bit less for women. Note the percentage of calories from fat: more than 77 percent for men and 72 percent for women. Given the BMIs just discussed, one can safely say based on this that eating a lot of fat did not make the participants fat.
The table below (click on it to enlarge) has some interesting health markers. Note that free fatty acids (FFAs) were elevated. This is to be expected, as these folks were burning fat for energy most of the time, and not as much glucose. The FFAs are not really “free”, but bound to a protein called albumin, which is abundant in human blood. FFAs yield large quantities of adenosine triphosphate (ATP), the main energy “currency” used by the body.
These levels of FFAs are also usually associated with mild ketosis, where ketones are produced by the body and used for energy. Unlike albumin-bound FFAs, ketones are soluble in water, and thus circulate freely through the blood. The mild ketosis experienced by the participants was possibly to the point where ketones showed in the urine. The article mentions this, and provides a measure of beta-HB (beta-hydroxybutyrate, a ketone body), which is elevated as expected, but does not provide urine or other blood ketone measures (e.g., blood acetone levels). Also note the fairly healthy fasting glucose levels, slightly higher in men than in women, but fairly low overall. Fairly healthy insulin levels as well; at the high end of what Stephan at Whole Health Source would recommend, but still significantly lower than the average insulin level in the U.S. at the time of the article's publication.
Finally, the table below (click on it to enlarge) shows lipids and a few other measures. Total cholesterol was on average a bit more than 278 mg/dL. LDL cholesterol was a bit higher than 188 mg/dL on average; high enough to make most doctors cringe today. Based on the means and standard deviations provided, we can estimate that about 16 percent of the participants had LDL cholesterol levels higher than 228.1 mg/dL. About 2.5 percent of the participants had LDL cholesterol levels higher than 268 mg/dL. And this is all after adhering to the diet for a relatively long period of time; even higher LDL cholesterol levels might have occurred right after adoption.
Yet average HDL cholesterol was a very high and protective 71.6 mg/dL. This high HDL and the relatively low triglycerides suggest a large-buoyant non-atherogenic LDL particle pattern.
Average HOMA(IR), a measure of insulin resistance, was a low 1.35 mU/mmol; strongly indicating, together with the relatively low fasting glucose levels, that the participants were far from being pre-diabetic, let alone diabetic.
Diabetes is a strong risk factor for cardiovascular disease, and many other health complications; much more so than elevated LDL cholesterol.
The Optimal Diet does not seem to be a diet for bodybuilders, but I would say that, overall, Peter at Hyperlipid has chosen a diet that makes some sense.
Reference:
Grieb, P. et al. (2008). Long-term consumption of a carbohydrate-restricted diet does not induce deleterious metabolic effects. Nutrition Research, 28(12), 825-833.
Sunday, April 11, 2010
The Friedewald and Iranian equations: Fasting triglycerides can seriously distort calculated LDL
Standard lipid profiles provide LDL cholesterol measures based on equations that usually have the following as their inputs (or independent variables): total cholesterol, HDL cholesterol, and triglycerides.
Yes, LDL cholesterol is not measured directly in standard lipid profile tests! This is indeed surprising, since cholesterol-lowering drugs with negative side effects are usually prescribed based on estimated (or "fictitious") LDL cholesterol levels.
The most common of these equations is the Friedewald equation. Through the Friedewald equation, LDL cholesterol is calculated as follows (where TC = total cholesterol, and TG = triglycerides). The inputs and result are in mg/dl.
LDL = TC – HDL – TG / 5
Here is one of the problems with the Friedewald equation. Let us assume that an individual has the following lipid profile numbers: TC = 200, HDL = 50, and trigs. = 150. The calculated LDL will be 120. Let us assume that this same individual reduces triglycerides to 50, from the previous 150, keeping all of the other measures constant. This is a major improvement. However, the calculated LDL will now be 140, and a doctor will tell this person to consider taking statins!
There is evidence that, for individuals with low fasting triglycerides, a more precise equation is one that has come to be known as the “Iranian equation”. The equation has been proposed by Iranian researchers in an article published in the Archives of Iranian Medicine (Ahmadi et al., 2008), hence its nickname. Through the Iranian equation, LDL is calculated as follows. Again, the inputs and result are in mg/dl.
LDL = TC / 1.19 + TG / 1.9 – HDL / 1.1 – 38
The Iranian equation is based on linear regression modeling, which is a good sign, although I would have liked it even better if it was based on nonlinear regression modeling. The reason is that relationships between variables describing health-related phenomena are often nonlinear, leading to biased linear estimations. With a good nonlinear analysis algorithm, a linear relationship will also be captured; that is, the “curve” that describes the relationship will default to a line if the relationship is truly linear (see: warppls.com).
Anyway, an online calculator that implements both equations (Friedewald and Iranian) is linked here; it was the top Google hit on a search for “Iranian equation LDL” at the time of this post’s writing.
As you will see if you try it, the online calculator linked above is useful in showing the difference in calculated LDL cholesterol, using both equations, when fasting triglycerides are very low (e.g., below 50).
The Iranian equation yields high values of LDL cholesterol when triglycerides are high; much higher than those generated by the Friedewald equation. If those are not overestimations (and there is some evidence that, if they are, it is not by much), they describe an alarming metabolic pattern, because high triglycerides are associated with small-dense LDL particles. These particles are the most potentially atherogenic of the LDL particles, in the presence of other factors such as chronic inflammation.
In other words, the Iranian equation gives a clearer idea than the Friedewald equation about the negative health effects of high triglycerides. You need a large number of small-dense LDL particles to carry a high amount of LDL cholesterol.
An even more precise measure of LDL particle configuration is the VAP test; this post has a link to a PDF file with a sample VAP test report.
Reference:
Ahmadi SA, Boroumand MA, Gohari-Moghaddam K, Tajik P, Dibaj SM. (2008). The impact of low serum triglyceride on LDL-cholesterol estimation. Archives of Iranian Medicine, 11(3), 318-21.
Yes, LDL cholesterol is not measured directly in standard lipid profile tests! This is indeed surprising, since cholesterol-lowering drugs with negative side effects are usually prescribed based on estimated (or "fictitious") LDL cholesterol levels.
The most common of these equations is the Friedewald equation. Through the Friedewald equation, LDL cholesterol is calculated as follows (where TC = total cholesterol, and TG = triglycerides). The inputs and result are in mg/dl.
LDL = TC – HDL – TG / 5
Here is one of the problems with the Friedewald equation. Let us assume that an individual has the following lipid profile numbers: TC = 200, HDL = 50, and trigs. = 150. The calculated LDL will be 120. Let us assume that this same individual reduces triglycerides to 50, from the previous 150, keeping all of the other measures constant. This is a major improvement. However, the calculated LDL will now be 140, and a doctor will tell this person to consider taking statins!
There is evidence that, for individuals with low fasting triglycerides, a more precise equation is one that has come to be known as the “Iranian equation”. The equation has been proposed by Iranian researchers in an article published in the Archives of Iranian Medicine (Ahmadi et al., 2008), hence its nickname. Through the Iranian equation, LDL is calculated as follows. Again, the inputs and result are in mg/dl.
LDL = TC / 1.19 + TG / 1.9 – HDL / 1.1 – 38
The Iranian equation is based on linear regression modeling, which is a good sign, although I would have liked it even better if it was based on nonlinear regression modeling. The reason is that relationships between variables describing health-related phenomena are often nonlinear, leading to biased linear estimations. With a good nonlinear analysis algorithm, a linear relationship will also be captured; that is, the “curve” that describes the relationship will default to a line if the relationship is truly linear (see: warppls.com).
Anyway, an online calculator that implements both equations (Friedewald and Iranian) is linked here; it was the top Google hit on a search for “Iranian equation LDL” at the time of this post’s writing.
As you will see if you try it, the online calculator linked above is useful in showing the difference in calculated LDL cholesterol, using both equations, when fasting triglycerides are very low (e.g., below 50).
The Iranian equation yields high values of LDL cholesterol when triglycerides are high; much higher than those generated by the Friedewald equation. If those are not overestimations (and there is some evidence that, if they are, it is not by much), they describe an alarming metabolic pattern, because high triglycerides are associated with small-dense LDL particles. These particles are the most potentially atherogenic of the LDL particles, in the presence of other factors such as chronic inflammation.
In other words, the Iranian equation gives a clearer idea than the Friedewald equation about the negative health effects of high triglycerides. You need a large number of small-dense LDL particles to carry a high amount of LDL cholesterol.
An even more precise measure of LDL particle configuration is the VAP test; this post has a link to a PDF file with a sample VAP test report.
Reference:
Ahmadi SA, Boroumand MA, Gohari-Moghaddam K, Tajik P, Dibaj SM. (2008). The impact of low serum triglyceride on LDL-cholesterol estimation. Archives of Iranian Medicine, 11(3), 318-21.
Friday, April 9, 2010
Full-fat Dairy for Cardiovascular Health??
[2013 update: a few colleagues and I have published a comprehensive review paper on the association between full-fat dairy consumption and obesity, metabolic health, and cardiovascular disease. You can find it here.]
I just saw a paper in the AJCN titled "Dairy consumption and patterns of mortality of
Australian adults". It's a prospective study with a 15-year follow-up period. Here's a quote from the abstract:
Contrary to popular belief, full-fat dairy, including milk, butter and cheese, has never been convincingly linked to cardiovascular disease. What has been linked to cardiovascular disease is milk fat's replacement, margarine. In the Rotterdam study, high vitamin K2 intake was linked to a lower risk of fatal heart attack, aortic calcification and all-cause mortality. Most of the K2 came from full-fat cheese.
From a 2005 literature review on milk and cardiovascular disease in the EJCN:
I just saw a paper in the AJCN titled "Dairy consumption and patterns of mortality of
Australian adults". It's a prospective study with a 15-year follow-up period. Here's a quote from the abstract:
There was no consistent and significant association between total dairy intake and total or cause-specific mortality. However, compared with those with the lowest intake of full-fat dairy, participants with the highest intake (median intake 339 g/day) had reduced death due to CVD (HR: 0.31; 95% confidence interval (CI): 0.12–0.79; P for trend = 0.04) after adjustment for calcium intake and other confounders. Intakes of low-fat dairy, specific dairy foods, calcium and vitamin D showed no consistent associations.People who ate the most full-fat dairy had a 69% lower risk of cardiovascular death than those who ate the least. Otherwise stated, people who mostly avoided dairy or consumed low-fat dairy had more than three times the risk of dying of coronary heart disease or stroke than people who ate the most full-fat diary. This result is an outlier, and also observational so difficult to interpret, but it certainly is difficult to reconcile with the idea that dairy fat is a significant contributor to cardiovascular disease.
Contrary to popular belief, full-fat dairy, including milk, butter and cheese, has never been convincingly linked to cardiovascular disease. What has been linked to cardiovascular disease is milk fat's replacement, margarine. In the Rotterdam study, high vitamin K2 intake was linked to a lower risk of fatal heart attack, aortic calcification and all-cause mortality. Most of the K2 came from full-fat cheese.
From a 2005 literature review on milk and cardiovascular disease in the EJCN:
In total, 10 studies were identified. Their results show a high degree of consistency in the reported risk for heart disease and stroke, all but one study suggesting a relative risk of less than one in subjects with the highest intakes of milk.
...the studies, taken together, suggest that milk drinking may be associated with a small but worthwhile reduction in heart disease and stroke risk.
...All the cohort studies in the present review had, however, been set up at times when reduced-fat milks were unavailable, or scarce.
The huge gap between glycemic loads of refined and unrefined carbohydrate-rich foods
I often refer to foods rich in refined carbohydrates in this blog as among the most disease-promoting agents of modern diets. Yet, when one looks at the glycemic indices of foods rich in refined and unrefined carbohydrates, they are not all that different.
The glycemic index of a carbohydrate-rich food reflects how quickly the food is digested and generate a blood glucose response. Technically, it is measured as the area under a two-hour blood glucose response curve following the consumption of a portion of the food with a fixed amount of carbohydrates.
A measure that reflects much better the underlying difference between foods rich in refined and unrefined carbohydrates is the glycemic load, which is the product of the glycemic index of a food by the carbohydrate content in a 100 g portion of the food.
The glycemic load is also the reason for one known fact among diabetics. If a diabetic person eats a very small amount of a high glycemic index food, he or she will have a relatively small increase in blood sugar. If that person consumes a large amount of the same food, the increase in blood sugar will be dramatic.
The table below (click on it to enlarge) shows the remarkable differences between the glycemic loads of foods rich in refined and unrefined carbohydrates. It was taken from an article co-authored by Loren Cordain, Michael R. Eades, and Mary D. Eades (full reference at the end of this post).
At the time of this post’s writing, the article from which the table above was taken had a solid number of citations to it; a total of 74 citations on Google Scholar’s database. It is an excellent article, which I highly recommend reading in full (the link to the online full text is at the end of this post).
What is the reason for the differences in glycemic loads?
The answer is that foods rich in unrefined carbohydrates, even those with a high glycemic index (such as potatoes), are also packed with a number of other things – e.g., micronutrients, fiber, water, and even some protein. An Irish (white) potato is 75 percent water. By comparison, cereal, without milk added, is about 1 percent water. You have to add a lot of whole milk to it to make it a bit healthier. And even unsweetened whole milk is about 5 percent sugar.
There was nothing even remotely similar to modern foods rich in refined carbohydrates in the diet of our Paleolithic ancestors. In fact, the types of food rich in refined carbohydrates shown on the table above are very recent, typically dating back to less than a hundred years ago. That is, they are so recent that it is unlikely that any of us have genetic adaptations to those types of food.
Once one’s glucose metabolism is seriously impaired, which seems to be associated with consumption over many years of refined carbohydrates and sugars (as well as some genetic predisposition, which may have evolved among some of our ancestors), then even the foods with high glycemic index and low glycemic load (e.g., potato) will lead to highly elevated glucose levels if eaten in more than very small amounts.
Insulin resistant individuals should avoid even foods with high glycemic index and low glycemic load, as well as any food that significantly increases their blood glucose levels after a meal, because highly elevated glucose levels are toxic to various tissues in the body. The longer those highly elevated serum glucose levels are maintained, the more damage is done; e.g., 2 hours as opposed to 30 minutes at 180 mg/dl. One reason why they are toxic is because they lead to high levels of protein glycation; this is a process whereby sugar binds to protein and “warps” it, impairing its functions.
Generally speaking, the more glycation is going on in our body, the more accelerated is the aging process.
Reference:
Loren Cordain, Michael R. Eades, Mary D. Eades (2003). Hyperinsulinemic diseases of civilization: More than just Syndrome X. Comparative Biochemistry and Physiology: Part A, 136, 95–112.
The glycemic index of a carbohydrate-rich food reflects how quickly the food is digested and generate a blood glucose response. Technically, it is measured as the area under a two-hour blood glucose response curve following the consumption of a portion of the food with a fixed amount of carbohydrates.
A measure that reflects much better the underlying difference between foods rich in refined and unrefined carbohydrates is the glycemic load, which is the product of the glycemic index of a food by the carbohydrate content in a 100 g portion of the food.
The glycemic load is also the reason for one known fact among diabetics. If a diabetic person eats a very small amount of a high glycemic index food, he or she will have a relatively small increase in blood sugar. If that person consumes a large amount of the same food, the increase in blood sugar will be dramatic.
The table below (click on it to enlarge) shows the remarkable differences between the glycemic loads of foods rich in refined and unrefined carbohydrates. It was taken from an article co-authored by Loren Cordain, Michael R. Eades, and Mary D. Eades (full reference at the end of this post).
At the time of this post’s writing, the article from which the table above was taken had a solid number of citations to it; a total of 74 citations on Google Scholar’s database. It is an excellent article, which I highly recommend reading in full (the link to the online full text is at the end of this post).
What is the reason for the differences in glycemic loads?
The answer is that foods rich in unrefined carbohydrates, even those with a high glycemic index (such as potatoes), are also packed with a number of other things – e.g., micronutrients, fiber, water, and even some protein. An Irish (white) potato is 75 percent water. By comparison, cereal, without milk added, is about 1 percent water. You have to add a lot of whole milk to it to make it a bit healthier. And even unsweetened whole milk is about 5 percent sugar.
There was nothing even remotely similar to modern foods rich in refined carbohydrates in the diet of our Paleolithic ancestors. In fact, the types of food rich in refined carbohydrates shown on the table above are very recent, typically dating back to less than a hundred years ago. That is, they are so recent that it is unlikely that any of us have genetic adaptations to those types of food.
Once one’s glucose metabolism is seriously impaired, which seems to be associated with consumption over many years of refined carbohydrates and sugars (as well as some genetic predisposition, which may have evolved among some of our ancestors), then even the foods with high glycemic index and low glycemic load (e.g., potato) will lead to highly elevated glucose levels if eaten in more than very small amounts.
Insulin resistant individuals should avoid even foods with high glycemic index and low glycemic load, as well as any food that significantly increases their blood glucose levels after a meal, because highly elevated glucose levels are toxic to various tissues in the body. The longer those highly elevated serum glucose levels are maintained, the more damage is done; e.g., 2 hours as opposed to 30 minutes at 180 mg/dl. One reason why they are toxic is because they lead to high levels of protein glycation; this is a process whereby sugar binds to protein and “warps” it, impairing its functions.
Generally speaking, the more glycation is going on in our body, the more accelerated is the aging process.
Reference:
Loren Cordain, Michael R. Eades, Mary D. Eades (2003). Hyperinsulinemic diseases of civilization: More than just Syndrome X. Comparative Biochemistry and Physiology: Part A, 136, 95–112.
Tuesday, April 6, 2010
Copper and Cardiovascular Disease
In 1942, Dr. H. W. Bennetts dissected 21 cattle known to have died of "falling disease". This was the name given to the sudden, inexplicable death that struck herds of cattle in certain regions of Australia. Dr. Bennett believed the disease was linked to copper deficiency. He found that 19 of the 21 cattle had abnormal hearts, showing atrophy and abnormal connective tissue infiltration (fibrosis) of the heart muscle (1).
In 1963, Dr. W. F. Coulson and colleagues found that 22 of 33 experimental copper-deficient pigs died of cardiovascular disease. 11 of 33 died of coronary heart disease, the quintessential modern human cardiovascular disease. Pigs on a severely copper-deficient diet showed weakened and ruptured arteries (aneurysms), while moderately deficient pigs "survived with scarred vessels but demonstrated a tendency toward premature atherosclerosis" including foam cell accumulation (2). Also in 1963, Dr. C. R. Ball and colleagues published a paper describing blood clots in the heart and coronary arteries, heart muscle degeneration, ventricular calcification and early death in mice fed a lard-rich diet (3).
This is where Dr. Leslie M. Klevay enters the story. Dr. Klevay suspected that Ball's mice had suffered from copper deficiency, and decided to test the hypothesis. He replicated Ball's experiment to the letter, using the same strain of mice and the same diet. Like Ball, he observed abnormal clotting in the heart, degeneration and enlargement of the heart muscle, and early death. He also showed by electrocardiogram that the hearts of the copper-deficient mice were often contracting abnormally (arrhythmia).
But then the coup de grace: he prevented these symptoms by supplementing the drinking water of a second group of mice with copper (4). In the words of Dr. Klevay: "copper was an antidote to fat intoxication" (5). I believe this was his tongue-in-cheek way of saying that the symptoms had been misdiagnosed by Ball as due to dietary fat, when in fact they were due to a lack of copper.
Since this time, a number of papers have been published on the relationship between copper intake and cardiovascular disease in animals, including several showing that copper supplementation prevents atherosclerosis in one of the most commonly used animal models of cardiovascular disease (6, 7, 8). Copper supplementation also corrects abnormal heart enlargement-- called hypertrophic cardiomyopathy-- and heart failure due to high blood pressure in mice (9).
For more than three decades, Dr. Klevay has been a champion of the copper deficiency theory of cardiovascular disease. According to him, copper deficiency is the only single intervention that has caused the full spectrum of human cardiovascular disease in animals, including:
The second reason you may not have heard of the theory is due to a lab assay called copper-mediated LDL oxidation. Researchers take LDL particles (from blood, the same ones the doctor measures as part of a cholesterol test) and expose them to a high concentration of copper in a test tube. Free copper ions are oxidants, and the researchers then measure the amount of time it takes the LDL to oxidize. I find this assay tiresome, because studies have shown that the amount of time it takes copper to oxidize LDL in a test tube doesn't predict how much oxidized LDL you'll actually find in the bloodstream of the person you took the LDL from (10, 11).
In other words, it's an assay that has little bearing on real life. But researchers like it because for some odd reason, feeding a person saturated fat causes their LDL to be oxidized more rapidly by copper in a test tube, even though that's not the case in the actual bloodstream (12). Guess which result got emphasized?
The fact that copper is such an efficient oxidant has led some researchers to propose that copper oxidizes LDL in human blood, and therefore dietary copper may contribute to heart disease (oxidized LDL is a central player in heart disease-- read more here). The problem with this theory is that there are virtually zero free copper ions in human serum. Then there's the fact that supplementing humans with copper actually reduces the susceptibility of red blood cells to oxidation (by copper in a test tube, unfortunately), which is difficult to reconcile with the idea that dietary copper increases oxidative stress in the blood (13).
The third reason you may never have heard of the theory is more problematic. Several studies have found that a higher level copper in the blood correlates with a higher risk of heart attack (14, 15). At this point, I could hang up my hat, and declare the animal experiments irrelevant to humans. But let's dig deeper.
Nutrient status is sometimes a slippery thing to measure. As it turns out, serum copper isn't a good marker of copper status. In a 4-month trial of copper depletion in humans, blood copper stayed stable, while the activity of copper-dependent enzymes in the blood declined (16). These include the important copper-dependent antioxidant, superoxide dismutase. As a side note, lysyl oxidase is another copper-dependent enzyme that cross-links the important structural proteins collagen and elastin in the artery wall, potentially explaining some of the vascular consequences of copper deficiency. Clotting factor VIII increased dramatically during copper depletion, perhaps predicting an increased tendency to clot. Even more troubling, three of the 12 women developed heart problems during the trial, which the authors felt was unusual:
Only a few studies have looked at the relationship between more accurate markers of copper status and cardiovascular disease in humans. Leukocyte copper status, a marker of tissue status, is lower in people with cardiovascular disease (22, 23). People who die of heart attacks generally have less copper in their hearts than people who die of other causes, although this could be an effect rather than a cause of the heart attack (24). Overall, I find the human data lacking. I'd like to see more studies examining liver copper status in relation to cardiovascular disease, as the liver is the main storage organ for copper.
According to a 2001 study, the majority of Americans may have copper intakes below the USDA recommended daily allowance (25), many substantially so. This problem is exacerbated by the fact that copper levels in food have declined in industrial nations over the course of the 20th century, something I'll discuss in the next post.
In 1963, Dr. W. F. Coulson and colleagues found that 22 of 33 experimental copper-deficient pigs died of cardiovascular disease. 11 of 33 died of coronary heart disease, the quintessential modern human cardiovascular disease. Pigs on a severely copper-deficient diet showed weakened and ruptured arteries (aneurysms), while moderately deficient pigs "survived with scarred vessels but demonstrated a tendency toward premature atherosclerosis" including foam cell accumulation (2). Also in 1963, Dr. C. R. Ball and colleagues published a paper describing blood clots in the heart and coronary arteries, heart muscle degeneration, ventricular calcification and early death in mice fed a lard-rich diet (3).
This is where Dr. Leslie M. Klevay enters the story. Dr. Klevay suspected that Ball's mice had suffered from copper deficiency, and decided to test the hypothesis. He replicated Ball's experiment to the letter, using the same strain of mice and the same diet. Like Ball, he observed abnormal clotting in the heart, degeneration and enlargement of the heart muscle, and early death. He also showed by electrocardiogram that the hearts of the copper-deficient mice were often contracting abnormally (arrhythmia).
But then the coup de grace: he prevented these symptoms by supplementing the drinking water of a second group of mice with copper (4). In the words of Dr. Klevay: "copper was an antidote to fat intoxication" (5). I believe this was his tongue-in-cheek way of saying that the symptoms had been misdiagnosed by Ball as due to dietary fat, when in fact they were due to a lack of copper.
Since this time, a number of papers have been published on the relationship between copper intake and cardiovascular disease in animals, including several showing that copper supplementation prevents atherosclerosis in one of the most commonly used animal models of cardiovascular disease (6, 7, 8). Copper supplementation also corrects abnormal heart enlargement-- called hypertrophic cardiomyopathy-- and heart failure due to high blood pressure in mice (9).
For more than three decades, Dr. Klevay has been a champion of the copper deficiency theory of cardiovascular disease. According to him, copper deficiency is the only single intervention that has caused the full spectrum of human cardiovascular disease in animals, including:
- Heart attacks (myocardial infarction)
- Blood clots in the coronary arteries and heart
- Fibrous atherosclerosis including smooth muscle proliferation
- Unstable blood vessel plaque
- Foam cell accumulation and fatty streaks
- Calcification of heart tissues
- Aneurysms (ruptured vessels)
- Abnormal electrocardiograms
- High cholesterol
- High blood pressure
The second reason you may not have heard of the theory is due to a lab assay called copper-mediated LDL oxidation. Researchers take LDL particles (from blood, the same ones the doctor measures as part of a cholesterol test) and expose them to a high concentration of copper in a test tube. Free copper ions are oxidants, and the researchers then measure the amount of time it takes the LDL to oxidize. I find this assay tiresome, because studies have shown that the amount of time it takes copper to oxidize LDL in a test tube doesn't predict how much oxidized LDL you'll actually find in the bloodstream of the person you took the LDL from (10, 11).
In other words, it's an assay that has little bearing on real life. But researchers like it because for some odd reason, feeding a person saturated fat causes their LDL to be oxidized more rapidly by copper in a test tube, even though that's not the case in the actual bloodstream (12). Guess which result got emphasized?
The fact that copper is such an efficient oxidant has led some researchers to propose that copper oxidizes LDL in human blood, and therefore dietary copper may contribute to heart disease (oxidized LDL is a central player in heart disease-- read more here). The problem with this theory is that there are virtually zero free copper ions in human serum. Then there's the fact that supplementing humans with copper actually reduces the susceptibility of red blood cells to oxidation (by copper in a test tube, unfortunately), which is difficult to reconcile with the idea that dietary copper increases oxidative stress in the blood (13).
The third reason you may never have heard of the theory is more problematic. Several studies have found that a higher level copper in the blood correlates with a higher risk of heart attack (14, 15). At this point, I could hang up my hat, and declare the animal experiments irrelevant to humans. But let's dig deeper.
Nutrient status is sometimes a slippery thing to measure. As it turns out, serum copper isn't a good marker of copper status. In a 4-month trial of copper depletion in humans, blood copper stayed stable, while the activity of copper-dependent enzymes in the blood declined (16). These include the important copper-dependent antioxidant, superoxide dismutase. As a side note, lysyl oxidase is another copper-dependent enzyme that cross-links the important structural proteins collagen and elastin in the artery wall, potentially explaining some of the vascular consequences of copper deficiency. Clotting factor VIII increased dramatically during copper depletion, perhaps predicting an increased tendency to clot. Even more troubling, three of the 12 women developed heart problems during the trial, which the authors felt was unusual:
We observed a significant increase over control values in the number of ventricular premature discharges (VPDs) in three women after 21, 63, and 91 d of consuming the low-copper diet; one was subsequently diagnosed as having a second-degree heart block.In another human copper restriction trial, 11 weeks of modest copper restriction coincided with heart trouble in 4 out of 23 subjects, including one heart attack (17):
In the history of conducting numerous human studies at the Beltsville Human Nutrition Research Center involving participation by 337 subjects, there had previously been no instances of any health problem related to heart function. During the 11 wk of the present study in which the copper density of the diets fed the subjects was reduced from the pretest level of 0.57 mg/ 1000 kcal to 0.36 mg/1000 kcal, 4 out of 23 subjects were diagnosed as having heart-related abnormalities.The other reason to be skeptical of the association between blood copper and heart attack risk is that inflammation increases copper in the blood (18, 19). Blood copper level correlates strongly with the marker of inflammation C-reactive protein (CRP) in humans, yet substantially increasing copper intake doesn't increase CRP (20, 21). This suggests that elevated blood copper is likely a symptom of inflammation, rather than its cause, and presents an explanation for the association between blood copper level and heart attack risk.
Only a few studies have looked at the relationship between more accurate markers of copper status and cardiovascular disease in humans. Leukocyte copper status, a marker of tissue status, is lower in people with cardiovascular disease (22, 23). People who die of heart attacks generally have less copper in their hearts than people who die of other causes, although this could be an effect rather than a cause of the heart attack (24). Overall, I find the human data lacking. I'd like to see more studies examining liver copper status in relation to cardiovascular disease, as the liver is the main storage organ for copper.
According to a 2001 study, the majority of Americans may have copper intakes below the USDA recommended daily allowance (25), many substantially so. This problem is exacerbated by the fact that copper levels in food have declined in industrial nations over the course of the 20th century, something I'll discuss in the next post.
Low fasting triglycerides: A marker for large-buoyant LDL particles
Small-dense LDL particles are particles that are significantly smaller than the gaps in the endothelium. The endothelium is a thin layer of cells that line the interior of arteries. Those gaps are about 25-26 nanometers (nm) in diameter. Small-dense LDL particles can contribute a lot more to the formation of atheromas (atherosclerotic plaques) in predisposed individuals than large-buoyant LDL particles.
Note that typically LDL particles are about 23-25 nm in diameter in most people, and yet not everybody develops atheromas. It is illogical to believe that evolution made LDL particles within those ranges of size to harm us, given the size of the gaps in the endothelium, unless you believe in something like this joke theory. There are underlying factors that make individuals much more prone to the development of atheromas than others.
One of those factors is chronic inflammation, which is caused by: chronic stress, excessive exercise (aerobic or anaerobic), and a diet rich in refined carbohydrates (e.g., white bread, pasta) and refined sugars (e.g., high fructose corn syrup, table sugar).
Can a standard lipid profile report tell me anything about my LDL particle pattern?
Yes, check you fasting triglycerides. If they are below 70 mg/dL, it is very likely that you have a predominance of large-buoyant LDL particles in your blood. That is, your LDL particle pattern is most likely Pattern A (see figure below, from: www.degomamd.com), the least atherogenic of the patterns identified by a Vertical Auto Profile (VAP) test. This test is more sophisticated than a standard lipid profile test, where the LDL cholesterol is typically calculated. For a sample VAP test report, see this PDF file from Atherotech.
So, you can get a rough idea about your LDL pattern type only by checking your fasting triglyceride levels on a standard lipid profile test report, if you cannot or do not want to have a VAP test done. The higher your fasting triglyceride levels are, above 70, the more likely it is that your LDL particle pattern is Pattern B, which is the most potentially atherogenic pattern.
Large-buoyant LDL particles often lead to high measured LDL cholesterol levels. This situation is analogous to that of water-filled balloons. If you have 10 balloons, each holding 0.5 L of water, then your total water amount is 5 L. If the same balloons are filled with 1 L of water each, then your total water amount is 10 L. That is, even though the number of LDL particles (analogous to the number of balloons) may be the same as that of a person with low LDL cholesterol, large-buoyant LDL particles have more cholesterol (water content in each balloon) in them, and lead to higher measured LDL cholesterol (total amount of water in the balloons) levels.
This leads to the counterintuitive situation where your LDL cholesterol levels go up, and your risk of developing cardiovascular disease actually goes down.
Also worth keeping in mind is that fasting triglyceride levels are strongly and negatively correlated with HDL cholesterol levels. The higher your fasting triglyceride levels are, usually the lower are your HDL cholesterol levels. The latter are also provided in standard lipid profile reports.
How do you decrease your fasting triglycerides?
A good way to start is to do some of the things that increase your HDL cholesterol.
References:
Elliott, W.H., & Elliott, D.C. (2009). Biochemistry and molecular biology. 4th Edition. New York: NY: Oxford University Press.
Lemanski, P.E. (2004). Beyond routine cholesterol testing: The role of LDL particle size assessment. CDPHP Medical Messenger, May 2004.
Note that typically LDL particles are about 23-25 nm in diameter in most people, and yet not everybody develops atheromas. It is illogical to believe that evolution made LDL particles within those ranges of size to harm us, given the size of the gaps in the endothelium, unless you believe in something like this joke theory. There are underlying factors that make individuals much more prone to the development of atheromas than others.
One of those factors is chronic inflammation, which is caused by: chronic stress, excessive exercise (aerobic or anaerobic), and a diet rich in refined carbohydrates (e.g., white bread, pasta) and refined sugars (e.g., high fructose corn syrup, table sugar).
Can a standard lipid profile report tell me anything about my LDL particle pattern?
Yes, check you fasting triglycerides. If they are below 70 mg/dL, it is very likely that you have a predominance of large-buoyant LDL particles in your blood. That is, your LDL particle pattern is most likely Pattern A (see figure below, from: www.degomamd.com), the least atherogenic of the patterns identified by a Vertical Auto Profile (VAP) test. This test is more sophisticated than a standard lipid profile test, where the LDL cholesterol is typically calculated. For a sample VAP test report, see this PDF file from Atherotech.
So, you can get a rough idea about your LDL pattern type only by checking your fasting triglyceride levels on a standard lipid profile test report, if you cannot or do not want to have a VAP test done. The higher your fasting triglyceride levels are, above 70, the more likely it is that your LDL particle pattern is Pattern B, which is the most potentially atherogenic pattern.
Large-buoyant LDL particles often lead to high measured LDL cholesterol levels. This situation is analogous to that of water-filled balloons. If you have 10 balloons, each holding 0.5 L of water, then your total water amount is 5 L. If the same balloons are filled with 1 L of water each, then your total water amount is 10 L. That is, even though the number of LDL particles (analogous to the number of balloons) may be the same as that of a person with low LDL cholesterol, large-buoyant LDL particles have more cholesterol (water content in each balloon) in them, and lead to higher measured LDL cholesterol (total amount of water in the balloons) levels.
This leads to the counterintuitive situation where your LDL cholesterol levels go up, and your risk of developing cardiovascular disease actually goes down.
Also worth keeping in mind is that fasting triglyceride levels are strongly and negatively correlated with HDL cholesterol levels. The higher your fasting triglyceride levels are, usually the lower are your HDL cholesterol levels. The latter are also provided in standard lipid profile reports.
How do you decrease your fasting triglycerides?
A good way to start is to do some of the things that increase your HDL cholesterol.
References:
Elliott, W.H., & Elliott, D.C. (2009). Biochemistry and molecular biology. 4th Edition. New York: NY: Oxford University Press.
Lemanski, P.E. (2004). Beyond routine cholesterol testing: The role of LDL particle size assessment. CDPHP Medical Messenger, May 2004.
Labels:
cardiovascular disease,
cholesterol,
HDL,
LDL,
research,
triglyceride,
VAP test
Sunday, April 4, 2010
Genetic clustering of metabolic disorders: Meet your relatives
As noted in this post, it is possible for a food-related trait to evolve to fixation in an entire population in as little as 396 years; not the millions of years that some believe are necessary for mutations to spread.
Moreover, evolution through fixation can occur in the absence of any selective pressure. That is, traits that are neutral with respect to fitness may evolve by chance, particularly in small populations. (A group of 100 individuals who made it to the Americas after a long and grueling trek would fit the bill.) This rather counterintuitive phenomenon is known as genetic drift (Hartl & Clark, 2007; Maynard Smith, 1998).
Fast evolution of traits certainly applies to polygenic traits, such as traits associated with nutrient metabolism. Polygenic traits are traits that are influenced by multiple genes, with those genes acting together to influence the expression of the trait.
Moreover, a mutation in one single pleiotropic gene (a gene that influences various traits) can lead to dramatic changes in interconnected phenotypic traits. This includes traits associated with complex processes involving multiple body tissues, such as glucose and fat metabolism.
Some disagree, arguing that complex traits need much longer to evolve. I wish I could be convinced of that; it would make our understanding of health issues and related predictions a lot easier. For example, we could zero in on Homo erectus as our target for an ideal Paleolithic diet.
Unfortunately, when you look around, you see people with food allergies, metabolic disorders, and other food- and lifestyle-related complications; and those problems cluster among people who seem to share recent common ancestors. Interestingly, in many cases those people do not look alike, in spite of sharing common ancestors.
For example, here in South Texas, it is clear that people from Amerindian ancestry (like me, although mine is from South America) are a lot more predisposed to diabetes than others. There are exceptions, of course; we are talking about probabilities here. Especially common here in South Texas are people with South and Central American Indian ancestry; less common but also represented are descendants of North American Indian tribes such as the Kickapoos.
Very recent food inventions, such as refined carbohydrates, refined sugars, omega-6-rich vegetable oils, and hydrogenated fats are too new to have influenced the genetic makeup of anybody living today. So, chances are, they are bad for the vast majority of us. Sure, a small percentage of the population may not develop any hint of diseases of civilization after consuming them for years, but chances are they are not going to be as healthy as they could be.
Other not so recent food inventions, such as olive oil, certain types of bread, certain types of dairy etc. may be better, in terms of overall health effects, for some people than for others. In fact, they may be particularly health-promoting for certain groups of individuals. The reason may be found in inherited metabolic traits. Learning about your ancestors could be helpful in this respect. The problem is that many people's ancestry is quite mixed; again, I give myself as an example - South American Indian, German, Italian, Portuguese ... and who knows what else.
Another, easier and perhaps more effective, way to figure out what particular foods, and in what quantities, may be healthy for you is to keep in touch with close and distant biological relatives; e.g., grandparents, parents, siblings, cousins (family gathering photo below from: www.lega.co.uk). It is likely that you share genes with them. If several of them developed a particular disease, and they consumed a lot of a certain type of food prior to that, then maybe that food should not be part of your diet.
This may also help you avoid making serious mistakes regarding health issues by acting too fast in response to laboratory test results. Relatives may share some quirky metabolic responses, which could be indicative of a disease at first glance and actually have no negative long term effects, and perhaps some positive ones.
For example, let us assume that a person, let us call her Mary, is in her early 50s and has been consuming a diet rich in refined carbohydrates and sugars for her entire life. Her fasting blood glucose looks pretty good at around 82 mg/dL.
Mary then adopts a diet that includes only vegetables and animal fat and protein. This new diet induces mild ketosis. She then notices that her fasting blood sugar is now 113 mg/dL, much higher than the previous 82 mg/dL. Mary’s doctor tells her that she may be pre-diabetic.
Mary knows that the change in diet was associated with the increase in fasting blood sugar, and reverts back to her diet rich in refined carbohydrates and sugars. Her fasting blood sugar goes down to 82 mg/dL, and she is happy. Her doctor congratulates her. However, she becomes obese and develops the metabolic syndrome in her late 50s, and several related diseases soon after.
Let us now look at a different scenario. After getting the 113 mg/dL fasting blood sugar reading on a mildly ketogenic diet, Mary talks to as many of her living relatives as she can. She asks many questions and finds out that a few of them were big meat and veggie eaters and had the same metabolic response. They are in their 60s and 70s and have no hint of diabetes. In fact, they are relatively lean and fairly healthy. She then sticks to her diet of only vegetables and animal fat and protein for life, and never develops the metabolic syndrome.
This fictitious case is based on the idea that low carbohydrate diets that induce mild ketosis may also induce physiological (not pathological) insulin resistance, leading to a version of the much talked about dawn phenomenon. This phenomenon, in this context, seems to be related to our good friend, but much maligned, palmitic acid. Several bloggers discussed it in excellent posts. Peter at Hyperlipid blogged about it here and here; Stephan at Whole Health Source blogged about it here.
Now, going back to keeping in touch with close and distant relatives. It is important to check your relatives’ lifestyle patterns as well, because diet is not everything, even though it is a major contributor to health outcomes. By lifestyle patterns I mean things like level and type of physical activity, sunlight exposure (which strongly influences vitamin D levels), and frequency and quality of social interactions (which reduce stress).
Regarding social interactions, it is worth noting that humans are highly social beings, and social isolation is almost universally detrimental to both mental and physical health.
References:
Hartl, D.L., & Clark, A.G. (2007). Principles of population genetics. Sunderland, MA: Sinauer Associates.
Maynard Smith, J. (1998). Evolutionary genetics. New York, NY: Oxford University Press.
Moreover, evolution through fixation can occur in the absence of any selective pressure. That is, traits that are neutral with respect to fitness may evolve by chance, particularly in small populations. (A group of 100 individuals who made it to the Americas after a long and grueling trek would fit the bill.) This rather counterintuitive phenomenon is known as genetic drift (Hartl & Clark, 2007; Maynard Smith, 1998).
Fast evolution of traits certainly applies to polygenic traits, such as traits associated with nutrient metabolism. Polygenic traits are traits that are influenced by multiple genes, with those genes acting together to influence the expression of the trait.
Moreover, a mutation in one single pleiotropic gene (a gene that influences various traits) can lead to dramatic changes in interconnected phenotypic traits. This includes traits associated with complex processes involving multiple body tissues, such as glucose and fat metabolism.
Some disagree, arguing that complex traits need much longer to evolve. I wish I could be convinced of that; it would make our understanding of health issues and related predictions a lot easier. For example, we could zero in on Homo erectus as our target for an ideal Paleolithic diet.
Unfortunately, when you look around, you see people with food allergies, metabolic disorders, and other food- and lifestyle-related complications; and those problems cluster among people who seem to share recent common ancestors. Interestingly, in many cases those people do not look alike, in spite of sharing common ancestors.
For example, here in South Texas, it is clear that people from Amerindian ancestry (like me, although mine is from South America) are a lot more predisposed to diabetes than others. There are exceptions, of course; we are talking about probabilities here. Especially common here in South Texas are people with South and Central American Indian ancestry; less common but also represented are descendants of North American Indian tribes such as the Kickapoos.
Very recent food inventions, such as refined carbohydrates, refined sugars, omega-6-rich vegetable oils, and hydrogenated fats are too new to have influenced the genetic makeup of anybody living today. So, chances are, they are bad for the vast majority of us. Sure, a small percentage of the population may not develop any hint of diseases of civilization after consuming them for years, but chances are they are not going to be as healthy as they could be.
Other not so recent food inventions, such as olive oil, certain types of bread, certain types of dairy etc. may be better, in terms of overall health effects, for some people than for others. In fact, they may be particularly health-promoting for certain groups of individuals. The reason may be found in inherited metabolic traits. Learning about your ancestors could be helpful in this respect. The problem is that many people's ancestry is quite mixed; again, I give myself as an example - South American Indian, German, Italian, Portuguese ... and who knows what else.
Another, easier and perhaps more effective, way to figure out what particular foods, and in what quantities, may be healthy for you is to keep in touch with close and distant biological relatives; e.g., grandparents, parents, siblings, cousins (family gathering photo below from: www.lega.co.uk). It is likely that you share genes with them. If several of them developed a particular disease, and they consumed a lot of a certain type of food prior to that, then maybe that food should not be part of your diet.
This may also help you avoid making serious mistakes regarding health issues by acting too fast in response to laboratory test results. Relatives may share some quirky metabolic responses, which could be indicative of a disease at first glance and actually have no negative long term effects, and perhaps some positive ones.
For example, let us assume that a person, let us call her Mary, is in her early 50s and has been consuming a diet rich in refined carbohydrates and sugars for her entire life. Her fasting blood glucose looks pretty good at around 82 mg/dL.
Mary then adopts a diet that includes only vegetables and animal fat and protein. This new diet induces mild ketosis. She then notices that her fasting blood sugar is now 113 mg/dL, much higher than the previous 82 mg/dL. Mary’s doctor tells her that she may be pre-diabetic.
Mary knows that the change in diet was associated with the increase in fasting blood sugar, and reverts back to her diet rich in refined carbohydrates and sugars. Her fasting blood sugar goes down to 82 mg/dL, and she is happy. Her doctor congratulates her. However, she becomes obese and develops the metabolic syndrome in her late 50s, and several related diseases soon after.
Let us now look at a different scenario. After getting the 113 mg/dL fasting blood sugar reading on a mildly ketogenic diet, Mary talks to as many of her living relatives as she can. She asks many questions and finds out that a few of them were big meat and veggie eaters and had the same metabolic response. They are in their 60s and 70s and have no hint of diabetes. In fact, they are relatively lean and fairly healthy. She then sticks to her diet of only vegetables and animal fat and protein for life, and never develops the metabolic syndrome.
This fictitious case is based on the idea that low carbohydrate diets that induce mild ketosis may also induce physiological (not pathological) insulin resistance, leading to a version of the much talked about dawn phenomenon. This phenomenon, in this context, seems to be related to our good friend, but much maligned, palmitic acid. Several bloggers discussed it in excellent posts. Peter at Hyperlipid blogged about it here and here; Stephan at Whole Health Source blogged about it here.
Now, going back to keeping in touch with close and distant relatives. It is important to check your relatives’ lifestyle patterns as well, because diet is not everything, even though it is a major contributor to health outcomes. By lifestyle patterns I mean things like level and type of physical activity, sunlight exposure (which strongly influences vitamin D levels), and frequency and quality of social interactions (which reduce stress).
Regarding social interactions, it is worth noting that humans are highly social beings, and social isolation is almost universally detrimental to both mental and physical health.
References:
Hartl, D.L., & Clark, A.G. (2007). Principles of population genetics. Sunderland, MA: Sinauer Associates.
Maynard Smith, J. (1998). Evolutionary genetics. New York, NY: Oxford University Press.
Subscribe to:
Posts (Atom)